How to Optimize Pre-Surgical Processes for Enhanced Outcomes with a FHIR-Enabled Data Activation Platform

While thousands of people continue to suffer the grave impacts of the COVID-19 pandemic, many have experienced hardship in other ways as a result of delays in needed medical and surgical interventions. Although postponing a majority of non-emergency surgeries was necessary for a time, hospitals need to be prepared as elective procedures are being reconsidered and might bounce back with a surge in cases.
According to a recent New York Times article, canceled elective surgeries, along with decreases in doctor’s visits and a decline in emergency department care, have accounted for almost $160 billion in lost revenue. Local and state health authorities have been issued guidelines by the Centers for Medicare and Medicaid Services on resuming elective surgeries in the post-COVID environment. However, for the most part, surgery is still being considered only when it’s necessary. Hospitals have to ensure they don’t allow a sudden surge in new infections, especially amongst medically fragile patients, while putting a strategy in place for patients whose conditions may significantly deteriorate while awaiting needed operations.
Variations in surgical outcomes
One of the major reasons healthcare costs are rising is the variation in clinical outcomes. A recent Reuters study found considerable variation in surgical outcomes, such as postoperative complications and “failure to rescue” rates, among hospitals within the same network. The 2019 study considered 87 hospitals, each tied to one of 16 networks affiliated with a U.S. News and World Report Honor Roll hospital. The data reviewed came from Medicare records for 143,174 patients who underwent either a colectomy, coronary artery bypass, or hip replacement operation between 2005 and 2014.
One of the most important metrics the researchers found was termed a “failure to rescue” rate, which measures how effectively hospitals cope with surgical complications. The Honor Roll “flagship” hospitals did better overall, with a 13 percent failure to rescue rate compared to the 15 percent seen in their affiliated hospitals. Similarly, the complication rates also varied between the affiliated and Honor Roll hospitals within their respective networks by as much as four times.
Although the findings of this study may not serve as conclusive proof that the care being delivered in affiliated hospitals was sub-par, it does highlight the fact that clinical variation is definitely something to be concerned about.
While little clinical variation exists for medical services overall, surgical procedures have received more negative press, given their high cost and the fact that they are usually planned medical services. Therefore, the expectation is that postoperative complications should be considered well in advance and avoided. That thought process leads to a seemingly simple solution: what if we made a concerted effort to reduce the variation associated with surgical procedures before they occur?
How can procedures for high-risk patients be optimized to minimize variation in clinical outcomes?
Today, there’s a pretty straightforward pathway to surgery. A patient, after consultation with their physician, contemplates surgery. There’s a preoperative assessment, which typically occurs in the weeks leading up to the procedure. However, any chance of improving the patient’s preparation for the operation is limited by one major factor: the ability to utilize the limited amount of time between first meeting the patient and the date of the procedure. During this time, opportunities to modify patient behavior beforehand and manage conditions that could lead to complications have been missed. There needs to be a process instituted routinely before the surgery: the pre-surgical optimization.
In most cases, benefits from surgery are derived exclusively from the primary reason for the procedure, such as the removal of a tumor. The harms, however, emerge from the unintended consequences of procedures, such as tissue trauma, infection, or blood clots. Pre-surgical optimization is a way that physicians, including anesthesiologists and specialists, nurses and care managers, can engage with patients before their planned surgical procedure. Pre-surgical optimization can help ensure that the patient is well-prepared in order to minimize the risk of perioperative complications.
For example, a patient with diabetes has a relatively high risk of postoperative complications. Uncontrolled diabetes can slow the healing of surgical wounds and put the patient at increased risk for infections, as well as kidney and heart problems. Similarly, obese patients and heavy smokers are at an increased risk of a number of medical and surgical complications, including wound infections, pneumonia, blood clots, sepsis, and heart attacks.
Achieving financial value through your pre-surgical optimization clinic
Optimizing patients before the surgery can help to generate considerable value in outcomes. For example, the association between diabetes and surgical site infections suggests a significant number of repeat operations and increased length of stay. With a detailed patient assessment and coordination between the surgeon, anesthesia team, primary care provider, specialists, and the care-coordination team, those undesirable outcomes can be minimized. Additionally, a similar impact would likely be seen on readmission rates. Optimized patients would be at lower risk of complications during these planned procedures and throughout the postoperative period.
Providers at UPMC Pinnacle in Harrisburg, Pennsylvania tried some pre-surgical optimization strategies with certain high-risk patients to reduce readmissions and complications. They found that creating an optimization clinic that enables coordination among care team members, provides patient education on how to optimize their modifiable risk factors, provides follow-up, and offers counseling and support up to the day of surgery, really helped. These strategies motivated patients to make lifestyle changes, such as reduced smoking, to control comorbidities because they were armed with the understanding that, by doing so, they can optimize their own outcomes. Within a year, a comparison of optimization clinic patients to all elective surgery patients revealed the following:
When comparing optimization clinic patients with comorbidities to all surgery patients with comorbidities, they found that:
The importance of an FHIR-enabled data platform to power your pre-surgical optimization clinic
Early assessment and engagement are best achieved by screening a patient’s risk profile as soon as possible after the decision is made for surgery. However, given that patient data is usually distributed across multiple systems such as EHRs, labs, radiology, outpatient clinics, hospitals, EDs, claims, and so on, it becomes necessary to integrate them first. Without unifying patient records, identifying clinical and social risk factors could be an excruciating task.
Integrating distributed patient data on an FHIR-enabled Data Platform equips healthcare organizations with a foundation. Powered by unified patient records, this foundation can be leveraged to identify which patients are at higher risk of complications, engage them, track and monitor their progress, provide support in optimizing modifiable risk factors, and deliver a comprehensive real-time view to physicians from the first visit until the day of surgery. Additionally, an FHIR-compliant platform can fast-track a secure exchange of data among different systems and ensure information is delivered where and when it’s needed to facilitate the optimization strategy.
With artificial intelligence and machine-learning algorithms running on the unified patient records, providers can quantify the risks that a patient might face and take the appropriate steps to minimize them. For example, if a patient prone to high blood pressure is about to undergo bypass surgery, their physicians and care managers working together can give proper medications, educate the patient, and monitor the response over time to bring the blood pressure under control. Similarly, the provider can work to adjust a diabetic patient’s insulin dose and plan for the appropriate pre- and postoperative dose adjustments. The optimization team can work with the patient on improving diet and exercise in order to maximize health conditions before the procedure. This concerted effort on the part of the team brings understanding and support for the patient, motivating them to make these changes in order to have a greater chance at a successful surgical outcome.
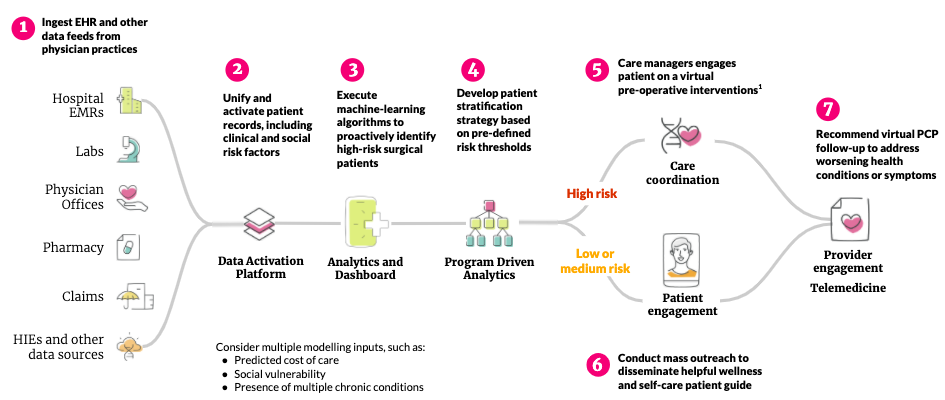
In the weeks leading up to the operation, the pathways for high-risk and low- or medium-risk patients become different. High-risk patients need to be engaged with preoperative interventions such as virtual consultations with specialists and specific changes in their medications, diet, or lifestyle. Patients designated medium-risk may follow a more conventional path but will still benefit from care managers reaching out to them with helpful wellness advice and self-care guidelines.
For the physician, it is important to have a real-time view of their patients. With telemedicine and virtual follow-up tools, physicians and care managers can check in on their preoperative patients and learn about worsening health conditions and new or recurring symptoms. Simply gaining more thorough insights into the patient’s health right at the point of care can make a significant difference down the road. Instead of diving deep into EHRs to retrieve information on the previous episodes, diagnoses, and other factors, a physician should be able to receive this information on the spot, while they’re talking to their patients. In the same way, they should be able to “chart as they consult,” ensuring that most of their time spent goes into assessing their patients.
Pre-surgical optimization opens up many opportunities to improve surgical outcomes and ensure adverse effects such as 30-day bounce-back admissions, difficulties obtaining postoperative follow-ups and medications, falls, infections and failure-to-rescue are minimized. Controlling outcome variations is something that can be achieved by redesigning care paths so that optimization teams encounter their patients well before the surgery and work together to help them make the right decisions about their treatment options and optimize their health before surgery.
To know more how a FHIR-enabled Data Activation Platform can help you in optimizing pre-surgical processes, get a demo.
For more updates, subscribe.
See the industry’s most advanced decision support system

