Reducing Network Leakage and Improve Physician and Patient Engagement Through a Comprehensive Referral Management Solution
Background
In the current referral management scenario, large scale providers are consistently struggling with:
- Network leakage – 10–20% out-of-network leakage
- Missing specialist details – 87% of out-of-network referrals are due to a lack of specialist details
- Patient unaware of referral status – 46% of faxed referrals never result in a scheduled appointment
- Incomplete referral loops – 40% of patients that follow through with appointments don't inform their PCP
As a result, many of our existing customers expressed interest in a solution that can improve the referral flow, reduce leakage, and enhance the physician and patient experience. Our Referral Management solution is an important step in that direction. The Solution is key for the larger provider networks that employ multiple physicians and a central referral team (CRT) that processes and transmits all the referrals in a centralized fashion.
Business Outcomes
Health systems typically have two primary business outcomes they are looking to drive through a referral management solution:
- For at-risk patients – preventing out-of-network referrals (leakage) to avoid losing control over care provided to the attributed patient, given they are on the hook for costs and quality for the entire attributed population, which impacts TCOC / shared savings. If there is a P4P arrangement, a health system might also be worried about the loss of revenue from patients leaving the system.
- For FFS (Fee-for-Service) patients – streamlining patient acquisition through PCPs for specialist visits, associated diagnostics, inpatient admissions, and other downstream revenue opportunities and proactively monitoring referral leakage from the PCPs to engage them in minimizing revenue leakage.
Proposed Workflow for End-to-End Referral Management
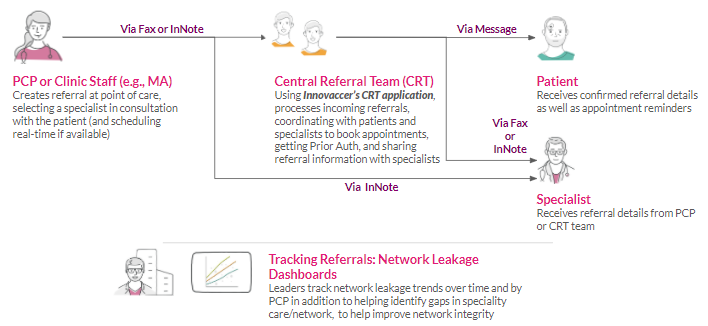
Development Approach
At the end of last year, we started building the MVP of our Referral Management solution with a solution for the CRT. A new cross-functional team was formed to develop and deliver an efficient CRT solution for our keystone customers.
Following true Agile principles, the team interacted with potential users frequently, helping the team identify and address the pain points and potential risks that should be mitigated in the initial phases. New solution wireframes were demoed to users in our initial discussions to help reduce the customer feedback loop. This lean approach instantly validated the product hypothesis and user experience that our design team had intended to create.
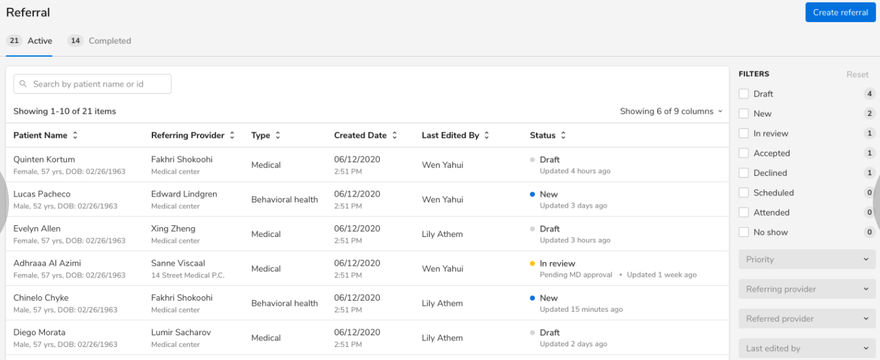
Key features of the solution
As a result of the iterative approach, we built a comprehensive solution with some key features, including:
- Worklist – group-based access to the worklist listing active and completed referrals/faxes with options to search, sort, and filter
- eFax capability – to receive new referrals and send processed referrals to specialists and patients through eFax
- Detailed referral workflow – to create new referrals, autofill patient / provider details, record referral information, input prior authorization number, document scheduled appointment details, etc.
- Patient insurance verification – to run real-time insurance verification before creating a referral to check patient eligibility for insurance plan
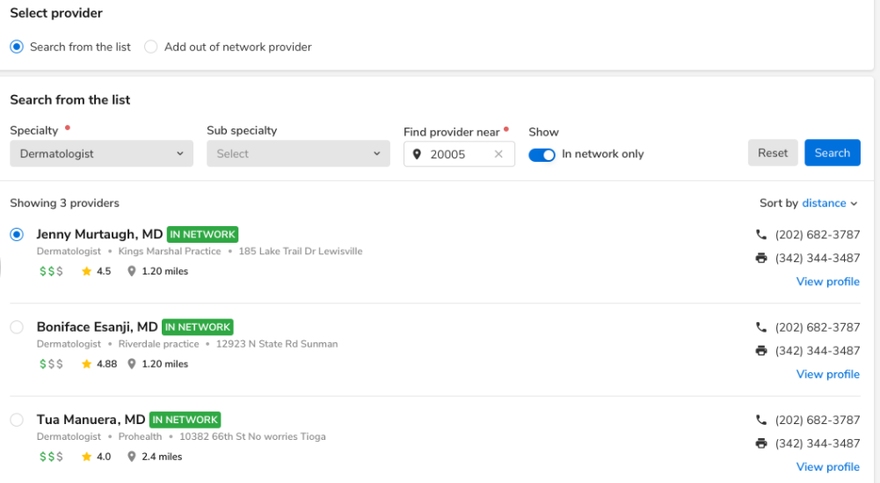
- In-network and out-of-network specialists – displays in-network providers sorted by distance and specialty, with an option to manually add out-of-network providers
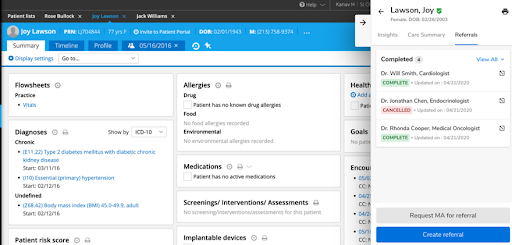
- Referral timeline – for a timeline view of the referral, displaying all status updates, activity on the referral
- Dashboards – a network leakage dashboard to track leakage trends by facility and provider, by month, by destination, by ICD codes, etc.; in addition to analyzing in-network and out-of-network options
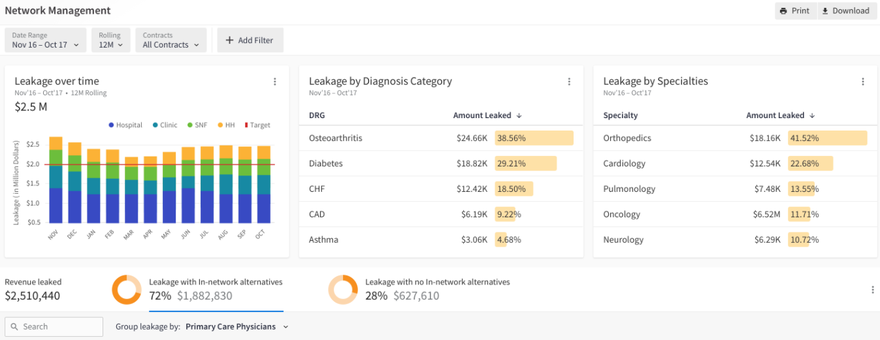
Key drivers of value / outcomes
- Reducing network leakage – monitor network performance / leakage through dashboards, optimize in-network referrals, identify causes of leakage
- Improving operational efficiency – advanced workflows, including sending and receiving faxes through eFax, enabling insurance verification, prefilling referral forms
- Improving quality of care – build your preferred specialist network, choose best-fit providers, promote in-network providers, ensure seamless sharing of clinical information
- Enhancing patient engagement – schedule appointments based on a patient’s availability, send automated appointment reminders, track referrals to close referral loops
What is coming next for referral management?
- Referrals at the point-of-care – allows providers (and their medical assistants) to create different types of referrals using our Physician Collaboration Tool (InNote), share with specialists, CRT, or patients, and track referral status
- Access to out-of-network providers – displays out-of-network providers within specific zip codes and provides additional details around cost and quality metrics
- Bidirectional sync with EMR – allows for information flow between the EMR and Referral Management applications, e.g., entering referral notes, medical data, investigations, etc.
- Appointment booking – EMR integration enables easy appointment booking into the provider’s schedule through the InNote and CRT applications
- TPA-based enhancements – runs Optical Character Recognition (OCR) on the incoming faxes to prefill the referral form, automating prior authorization workflows
- Additional worklist functionality – provides push notifications when a fax is received, allows the assigning and re-assigning of faxes and tasks, automatically places a referral that needs attention at the top of the list
- Business rules – segments new referrals based on predefined rules to identify the next action and status, e.g., generates the correct form layout, pre-selects a specialist
Why Innovaccer for Referral Management?
We offer key differentiators that add additional value and distinguish our solution from that of competitors -
- Comprehensive solution with broad functionalities – offering differentiating factors like real-time insurance verification, OCR, e-fax capability, eConsults, business rules
- Catering to multiple personas – solving the use cases / requirements of providers, CRT, medical assistants, population health managers, etc., by offering integrated provider and CRT workflows
- State-of-the-art dashboards – allowing the tracking of referrals / leakage at provider, facility, and ACO levels
- Deep understanding of the healthcare industry – delivering our expertise in working with 25K+ providers across 1,000+ geographies and knowledge of the nuances of referral management workflows
- Seamless integration with other applications – our application integrates with patient relationship management and provider point-of-care applications to create a panoramic view for the provider
See the industry’s most advanced decision support system

