Time to care for payer care management

The pandemic set a lot of things into motion in the healthcare system. Gaps in care delivery that seemed imperceptible, now seem to be staring the stakeholders right in their faces. Reforms such as telemedicine that appeared to be taking place slowly quickly changed their pace of adoption. To adapt to the changing healthcare landscape, payers need to work to optimize and improve care management solutions to adapt to the changing healthcare landscape.
It’s estimated that the healthcare management market will be worth $20 billion by 2023. Payers—who are as responsible for care management and delivery as provider networks—must focus on care management to improve quality, make better value-based decisions, reduce costs, and, most importantly, improve member satisfaction.
6 Ways Payers Can Improve Efficiency
Payers can improve efficiency in several areas. For example, many care management programs focus on preventing medical events without helping members consult efficient, high-quality doctors or select the most appropriate site of clinical care. With the following measures, payers can resolve issues and improve care management to achieve better results for members:
- Perform member segmentation
Each member archetype has unique needs. Segment them and then identify the areas in which the best quality care can be provided at the most appropriate costs rather than driving the same source of value for all members under a plan.
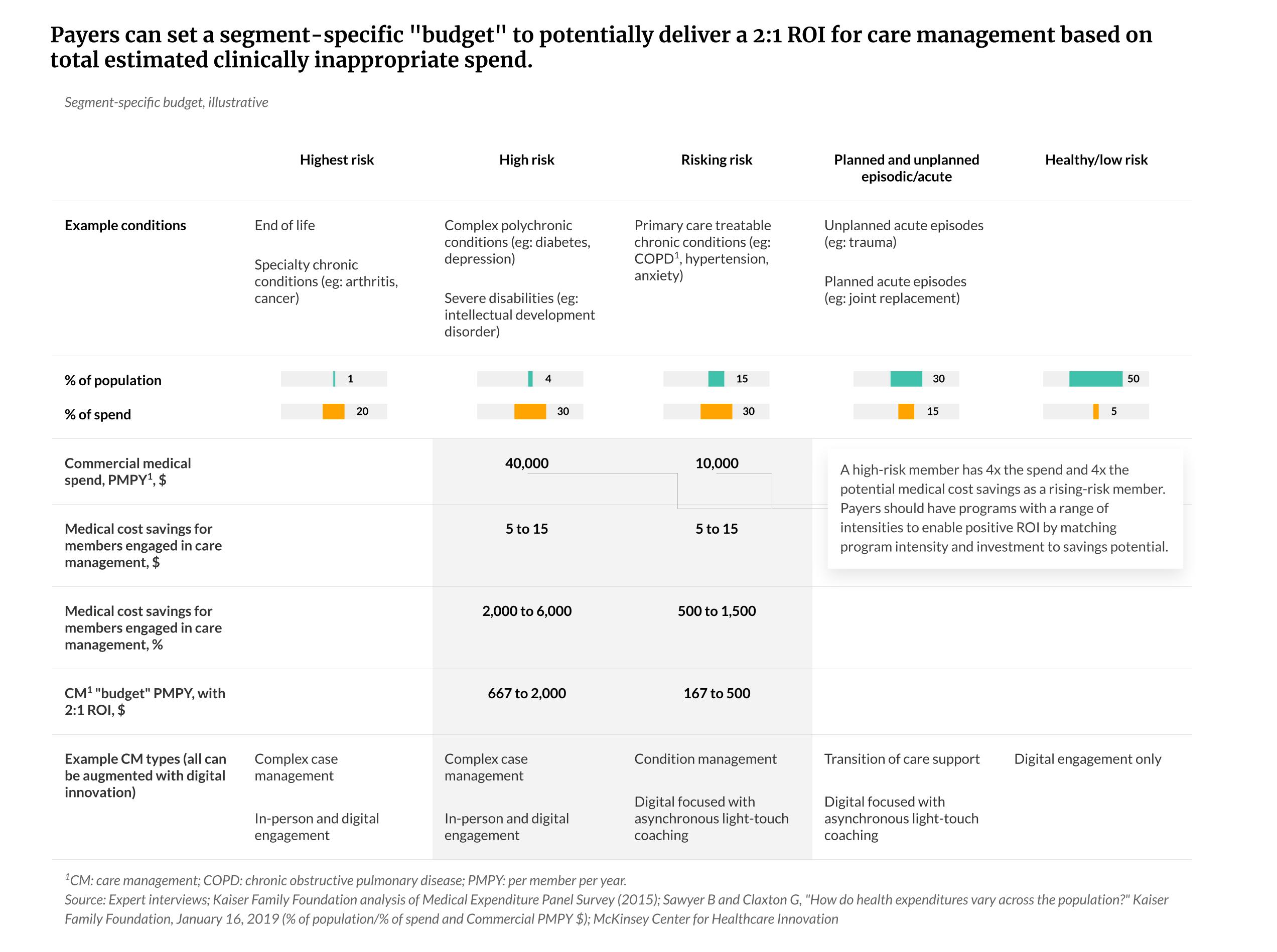
- Adjust the intensity of care management
Payers often focus on total spend rather than clinically appropriate spending. To reduce unnecessary spending, the intensity of care management should be tailored to the needs of target populations and manage and deliver care efficiently. This can lower costs and increase return on investment (ROI). Such a system allows high- and low-risk patients to access adequate care at appropriate costs.
- Digitize and automate
Many care management and delivery processes are still performed manually such as calling members, assigning cases to care managers, etc. However, repetitive tasks can easily be automated through digital solutions. For example, automated algorithms can prioritize cases based on data curated on the right data platform.
- Find the right time for member engagement
Proper timing of communications is vital. If the receiving member is engaged at a time when they are unlikely to be receptive. A high-risk patient who frequently communicates with providers may not be receptive to engagement, while a member who has just been discharged is more likely to respond to engagement initiatives. Reaching out at the right time is the key to success here.
- Bring consumerism to engagement
Healthcare organizations have historically failed to treat members like consumers. Take a leaf out of other industries where consumer engagement strategies have advanced far beyond what is currently done in healthcare. Microtargeting and personalization can help care management programs deliver more value to members. An engagement-first approach that puts the needs of consumers at the centre makes the offering more attractive and simplifies communication between care managers and members to promote required behavioral changes in patients. Moreover, psychometric segmentation of members can help make engagement more effective.
- Improve analytics for data-driven decision-making
Payers should gather updated member and provider data to improve member identification and impact care management for the target populations. Decisions based on insights from member data can impact care delivery. Even basic tasks such as updating contact information can help payers have access to multiple communication channels that can be leveraged for member engagement. For example, using a cell phone number instead of a landline number to contact a member can reduce unnecessary calls if members are not at home (or no longer have a landline).
Member-Centric Care Management
Payers need to refine their care management programs and strategically work to make them more member-centric. Care management is an area of enormous opportunity for payers, especially given the impacts of COVID-19.
To learn how your care management programs can improve member satisfaction and care quality, get a demo of the industry’s most comprehensive healthcare data platform for payers.
Subscribe for more updates on the shifting healthcare landscape.
See the industry’s most advanced decision support system