Five Biggest Challenges Health Systems Face While Integrating Digital Solutions With the Health IT Ecosystem

Innovation in healthcare digital technologies has exploded in recent years. The increasing maturity and accessibility of scalable and cost-effective cloud infrastructure have democratized innovation beyond major EHR vendors and introduced new players in the care ecosystem. The wearable medical devices market has further grown to cover a third of the US adult population in 2023, leading to the emergence of new app platforms for innovation and riding the wave of remote care. Moreover, the pandemic further spurred investment in this sector, and what we have now is a digital health market that has nearly doubled in size since 2019. In response to this growth, the global healthcare interoperability market is also predicted to climb to $5.7 billion by the end of 2026, as per a recent research report.
New solutions are arriving rapidly and must be woven into the already-complex digital tapestry across the care ecosystem. Decision support tools must overlay or embed within medical record systems to empower physicians and care teams to make data-driven decisions. Patient-generated home device data must be reconciled with decision support and EHR documentation to enrich patient profiles with real-time data. Life sciences solutions, patient mobile apps, and telemedicine solutions must operate on an independent data cloud to run data operations at scale. But, healthcare data and workflows today are siloed, if not more so, than ever before.
As new technologies create and manage more data, healthcare interoperability and data sharing are going to become increasingly critical for delivering effective healthcare. True interoperability has the potential to revolutionize the way care is delivered and received and must be a critical component of digital transformation strategy in today’s climate but it remains a significant challenge. IT leaders, developers, and engineers working in the healthcare technology space deal with a complex landscape of regulations, standards, and technologies to develop solutions that can effectively share and exchange information.
Connected Digital Solutions: What's Holding Us Back?
While IT leaders and providers are thinking about how to successfully enable a strategy to leverage interoperability, they face several challenges in their journey to connect digital solutions to their healthcare IT ecosystem.
Digital health engineering leadership in turn must ensure that they are following the best practices and avoiding common pitfalls early in the ideation and product discovery stage. They also need to ensure that their solutions are well-positioned to successfully achieve interoperability with EHRs and with their customers’ technology environment.
Let’s deep dive into the top five interoperability and data exchange issues that digital health technology leaders, health system IT leaders, and their teams face while building and implementing EHR-integrated solutions.
- Lack of EHR Standardization
One of the biggest challenges facing developers and engineers is the lack of standardization across various EHR systems, especially when sending data back to the EHR. Fast Healthcare Interoperability Resources (FHIR) APIs have revolutionized data access from EHR systems. FHIR, however, doesn't support writing data back to EHRs.
EHRs—the patient’s system of record—is not the place to dump and crunch all your data. We must be good stewards of the patient record and make sure that high-quality insights are written back into EHR workflows.
In terms of writing data, the majority of EHR vendors are still heavily dependent on native APIs or HL7 interfaces. Needless to say, these standards have implementation-level customizations as well, such as Z-segments and custom mappings for HL7 or different profiles in the case of FHIR. Building a robust generic solution for writing data is a time-consuming task and requires expertise in the workings of individual EHRs.
Beyond the data transmission layer, each EHR system has its own unique structure and data format, making it difficult to develop solutions that can work in a generalized way across multiple platforms. For example, certain systems will format content with rich text, some with HTML, and others cannot format content at all beyond plain text. Ensuring consistency of content requires a deep understanding of these variances at the system level. More complex concepts, such as care pathways, care plans, and appointment workflows exhibit deep divergence across the industry which requires that the developer chooses between standardization of all systems and optimization of each system.
FHIR has dramatically improved standardization; however the persistent need to optimize on a per-EHR basis can lead to increased development costs, a longer time to market, and high maintenance burden. In today’s highly competitive market, solution architects must implement highly optimized solutions on a per-EHR basis or partner with a middleware that is up to the challenge. IT leaders must recognize the limitations of generalized approaches and support vendors with a demonstrated granular understanding of their EHR systems.
- Limited Access to Patient Data
Data is the key to providing meaningful insights and improving patient outcomes. Due to limitations at source to exchange data and the lack of data from sources such as specialist clinic visits and insurance claims, an EHR can have limited data. This can lead to data incompleteness and accuracy-related issues with the available data due to manual data entry.
In addition, with each new data source comes a new data silo. A patient’s social determinants reside in one place, their sequenced genome may be saved on a proprietary cloud, and their RPM (remote patient monitoring) devices and wearables are generating data at staggering rates, with concepts like continuous blood pressure monitoring nearing the horizon.
These data sources, when integrated, can provide complete visibility for the continuum of care. But when left disintegrated, they represent a massive burden on development costs, increased risk due to system complexity, and susceptibility to duplication of data.
Digital health companies planning to leverage data from disparate silos, be it claims data, clinical data, or home device data, will need to manage multiple point-to-point integrations with several different systems, each with its own special transmission mechanism or API and points of failure. As a result, the IT ecosystem at most health systems today is less like a well-organized hub and spoke model and more like a spiderweb of interconnected interfaces and API requests.
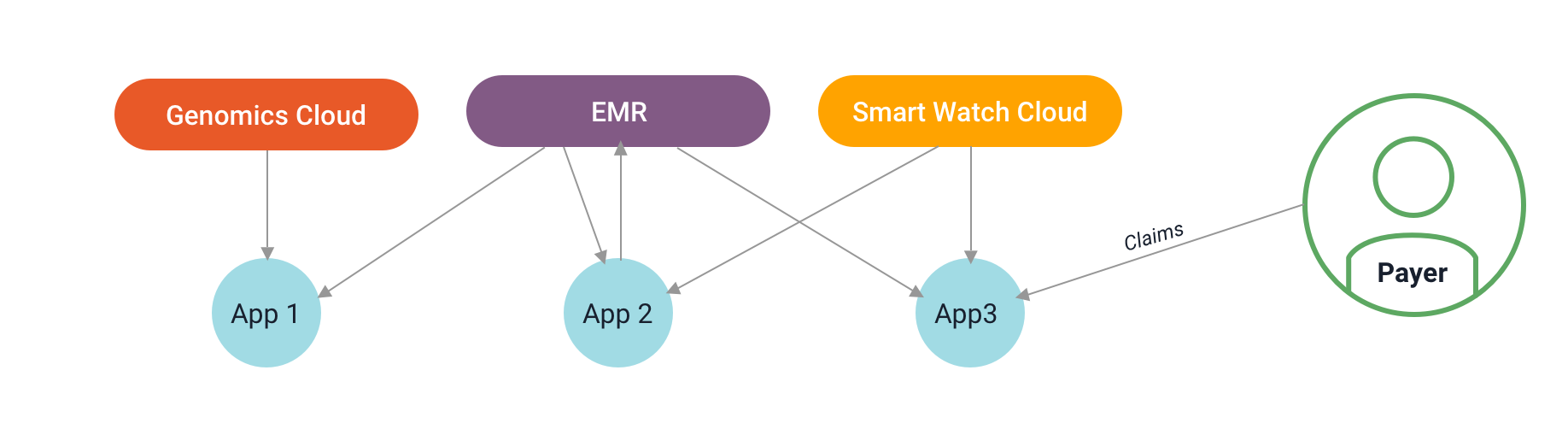
HIT systems without a data lake
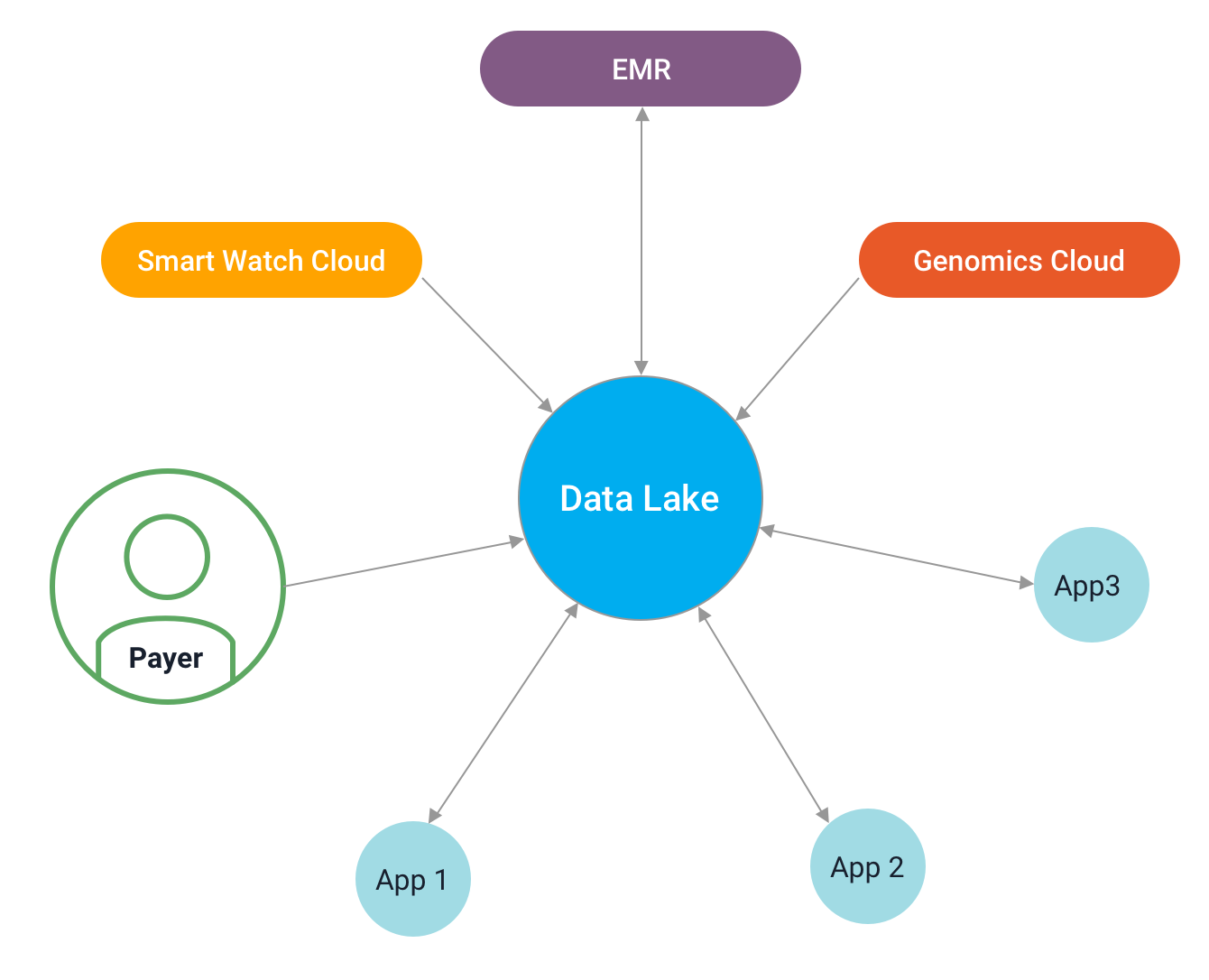
HIT systems with a data lake
The fact that data is stored in silos across multiple systems makes it unlikely that any data transformation operation supported by interoperability can be successful unless the patient's data is fully integrated.
- Inconsistent User Experiences
Creating an intuitive and user-friendly interface for EHR-integrated solutions is crucial for healthcare providers to adopt and effectively use the solution. The user experience must take into account the specific needs and workflow of providers and their care teams, which can be a complex and time-consuming task. Look no further than the physician burnout crisis. Providers don’t want a solution that takes more time away from their patient interactions. It is unlikely that any solution will succeed if it amplifies only the negative elements of the physician experience.
Furthermore, we need to reduce the administrative burden for providers. There shouldn't be a separate login process or a system that complicates existing workflows with an integrated solution. In addition to the login wall and the policies for usernames and passwords, data silos come with their login walls. In this respect, SMART-on-FHIR presents an opportunity by leveraging the EHR as a single sign-on identity provider. Still, adoption has been limited so far in digital health applications. This can be attributed to a lack of knowledge on the vendor side, as well as limitations in the technology infrastructure on the EHR side, including reliance on outdated browser technology (IE10 and IE11).
Equally important is the need to ensure as much design consistency as possible across different EHR systems, so that these user-facing solutions are seamless when operationalized. Even if a solution is perfectly integrated from a workflow and data perspective, the odds are higher that the design principles and training aspects will vary greatly from the EHR and other integrated apps. User experience design and training best practices must be advocated and adopted with equal importance as the industry does around FHIR for data transmission.
- Securing PHI and PII
Developing interoperable digital health solutions requires a broad strategy to safely manage data due to the inherent risks in working with sensitive patient information.
For Health IT leadership, every new onboarded digital solution represents another link in the data security chain, and the weakest link will determine if and when a data breach or data exposure occurs. When digital solutions talk to different EHRs, a single exposed password or credential can have a domino effect.
One of the best ways that an application can reduce the risk of exposure is by storing as little data as possible.
In the past, when HL7 interfaces and C-CDA exchange ruled interoperability, this was not possible as all applications would need to maintain their own private data store to power application functions. With the advent of FHIR, we are much closer to a future where many applications can become stateless, running synchronously along with the API. Imagine your applications having no persistent PII or PHI and simply requesting the data they need directly from the API, at the moment they need it.
We see many applications attempt to do just that, only to run into heavy latency issues with EHR FHIR APIs, or run into pagination of hundreds of vitals deriving from a patient’s ICU visit. With many EHRs having built their FHIR APIs as a facade over legacy service, high latency remains to be a recurring issue. This leads to poor user experiences and perceived slowness, as functionality relying on FHIR API data inherits the lag time of the API.
A data lake serving as an intermediary between the EHR and client applications can be a good choice for enabling stateless, synchronous application behavior and reducing data exposure risk.
- Keeping Up With the Latest Tech in the Industry
EHR marketplaces and technologies are constantly evolving and developers and health IT leadership must be aware of the latest updates and changes to ensure that their solutions remain compatible and effective. This can be a significant challenge as it requires ongoing maintenance, development efforts, and unexpected IT costs. This can be a full-time job in itself and require breaking changes in the system at times. Failure to do so can lead to compatibility issues and compromised effectiveness of the solution.
This problem is compounded when organizations build systems optimized to the unique constraints of each particular EHR. Although a superior result may be achieved in this way, the product becomes exposed to any sudden changes in EHR functionality or policy, multiplied by each EHR that they are directly integrated with.
Health IT leaders must also pay very close attention to government-led initiatives and trends. The Office of the National Coordinator for Health Information Technology (ONC), for example, has taken a decisive role in enforcing the adoption of FHIR APIs to standardize data exchanges with EHRs. CMS largely defines what payers must conform to CMS-0057-P and its implications for broader payer data access. These initiatives directly impact what kind of capabilities data sources will offer and therefore should be a key input to drive solution roadmaps.
Providing feedback and participating in standards development and regulatory thought process is, therefore, a crucial element to operating a leading-edge interoperability strategy. More than a full-time job, this task often is neglected and solution developers frequently find themselves reacting to, instead of driving, industry initiatives in interoperability.
The Road Ahead
Integrating external applications into EHR systems is a complex task that requires a deep understanding of data structures, formats, and regulatory standards. But with the right approach IT leaders, developers, and engineers can help pave the way for a more connected and efficient healthcare system that can provide whole-person care. Additionally, working with partners and vendors that have proven expertise in developing interoperable solutions powered by enterprise data models on purpose-built healthcare data platforms can have a significant impact on reducing the time to value for providers.
Putting the Patient Back at the Center
For patients to have a great experience across their care journey requires real-time data access and sharing between disparate systems and easy access to personal health information. Interoperability is at the heart of the patient’s care journey. When healthcare systems can talk to each other and share data seamlessly, providers can truly put patients at the center of high-quality care.
A healthcare data integration platform powers data exchange, access, and use. It unifies data from numerous sources into a single patient record and uses matching logic—powered by an extendable unified data model—to recognize and reconcile data for each patient.
Digital Health Platforms, like Innovaccer’s #1 Best in KLAS Data & Analytics platform, provide a standard out-of-the-box offering that works with and talks to any EHR and external system. The platform sends data to different EHRs using standard exchange protocols (like FHIR and HL7) with minimal additional development work.
We partner with providers to eliminate real-life care delivery challenges like duplicate documentation scenarios and a lack of data visibility across systems, providing back-and-forth data flow and real-time care management data integration. Innovaccer also has a roadmap packed with capabilities that put interoperability—and patients—front, and center. We believe simplicity, enabling data exchange between all EHRs, and improving every step of the patient journey will improve overall care quality and experiences.
To learn more about how your organization can also deliver excellent care experiences leveraging interoperability, click here for a free demo and consultation.