How can Payers Leverage Digital Chart Retrievals Using a FHIR-enabled Data Activation Platform

Every year health plans are required to gather and report their patient data for evaluation based on the Healthcare Effectiveness Data and Information Set (HEDIS®), a set of performance metrics established by the National Committee for Quality Assurance (NCQA). Until 2019, 90 percent of the health plans used HEDIS to measure their performance.
For on-going improvement in healthcare quality, NCQA updates the technical specifications continuously. In 2019, there were a total of 92 measures across multiple domains of care. Updating the data accumulation and reporting process to accommodate the ever-changing metrics is challenging. Health plans need to ensure that their medical chart retrieval process is optimized and relevant healthcare stakeholders can access the data they need quickly.
Along with reporting requisites, the chart retrieval process also has a significant role in claims processing. Payers need to evaluate each claim they receive, taking into account the patient's complete health history and the medical records to make the right payment decision. Any discrepancy can lead to unnecessary costs or wrongfully denied claims and dissatisfaction among the members. Tracking, managing and ensuring the availability of the medical records at the right place, at the right is critical.
Need for an Efficient Chart Retrieval Process
Payers invest millions of dollars and countless hours retrieving charts and relevant clinical data, taking as much as 20 days. Acquiring these charts via a third party vendor is expensive and could cost as much as $12 per chart. Obtaining relevant clinical records, reviewing them, and extracting reliable results from them is already a complicated process, further tangled by the lack of interoperability among EHRs.
Then, of course, is the need to review the charts to identify gaps in care and provide member-level decision support to providers at the point of care. Topping it all, HEDIS measures and CMS STAR ratings are governing the performance of payers, making it important to retrieve charts effectively, not to mention rapidly.
The best possible way to simplify the process is to enhance connectivity among healthcare data systems and automate the chart retrieval processes. The biggest challenge is that the data systems in healthcare are not currently interoperable. If simple, yet robust connection mechanisms are leveraged, the time to acquire data could be greatly reduced. Whether it be patient charts, physician notes, or lab orders, all of these elements must be brought together on a FHIR-enabled Data Activation Platform to create a unique and longitudinal record for each member.
Leveraging FHIR-enabled Data Activation Platform for Medical Chart Retrievals
Developing an efficient medical chart retrieval process is essential to optimize the cost functions and boost membership. Payers need to look for a chart retrieval system that allows end-to-end processing and workflow automation. Health plans also need analytics features that can help with quality improvement and revenue forecasting to gain a competitive edge as the average STAR Ratings for Medicare Advantage in 2020 is phenomenally high, 4.16 out of 5 stars.
To assist payers in dealing with increasing manual processes and achieving better STAR ratings, Innovacer's FHIR-enabled Data Activation Platform supports automated chart retrieval and review. The chart retrieval offering is purpose-built for payers to help them gain control over full-breadth of data and focus on what is important to them.
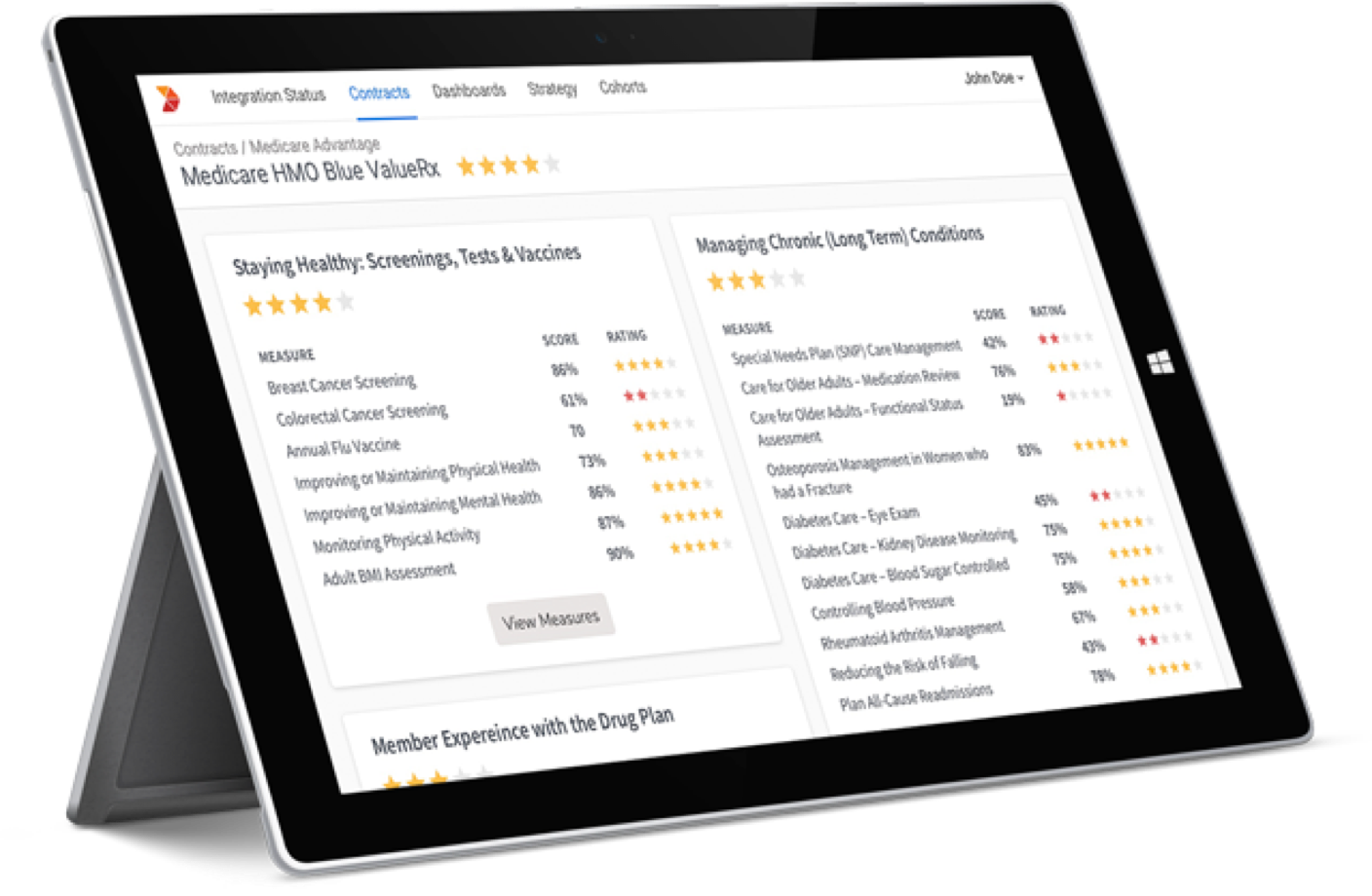
With API-based connectivity, 200+ pre-built connectors, and scalable architecture, the FHIR-enabled Data Activation Platform can capture a breadth of healthcare data and enable quicker access to clinical data and chart retrievals, at less than half the costs incurred using manual processes. Additionally, the payers can go deep down into healthcare coding standards and ensure appropriate care actions.
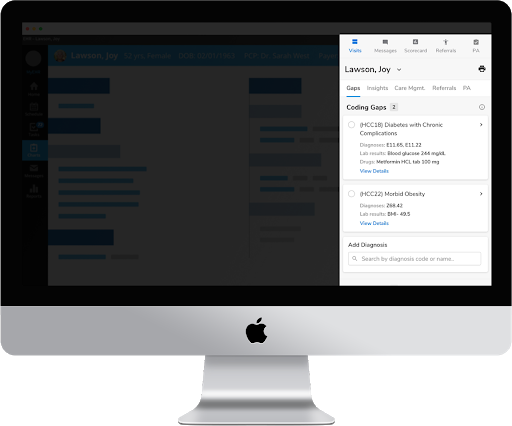
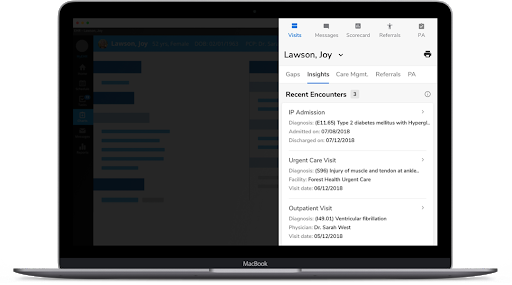
Using FHIR-enabled Data Activation Platform's point-of-care alerts, payers can engage with physicians to share and close gaps in care, including risk factors, coding gaps, and outstanding measures. Combined with automated chart retrieval, payers can leverage the FHIR-enabled Data Activation Platform to transform their existing processes and generate more cost savings.
The Road Ahead
Although many payer organizations have employed a data warehouse or analytics to analyze patient records and enhance STAR ratings, these approaches need to be scaled up to address future healthcare requirements.
Payers need a more comprehensive view of population health that can help them adopt a better outcomes-driven approach. Automated chart retrievals and reviews will be pivotal in driving a faster time-to-value and leading healthcare to an era of data-powered outcomes.

.svg)


.png)



.png)



.avif)


.png)
.png)
.png)




.svg)
.svg)

.svg)

