How can Healthcare Organizations Achieve Seamless Interoperability with the FHIR-enabled Data Activation Platform

U.S. healthcare has made remarkable progress in facilitating interoperability. In a survey of hospitals and health systems, 69 percent of respondents said that they are able to share data within their own health system efficiently. In order to deliver better care and improve outcomes, most healthcare providers were quick to take measures to establish internal interoperability. However, when it came to sharing health data with other providers, payers and patients, the adoption of interoperability-driving technologies has been sluggish.
“Healthcare providers and technology developers may have powerful economic incentives not to share electronic health information and to slow progress towards greater data liquidity,” said Don Rucker, MD, national coordinator for health I.T.
Almost 18 percent of the country’s GDP goes to the healthcare sector and despite the high expenditure, the quality of care is still unsatisfactory. U.S. healthcare ranks at or near the bottom in almost every measure of comparative quality among other developed nations. The only way to overcome the healthcare rut is by making stakeholders unite and share health data to improve the overall quality of care delivery, reduce barriers and boost population health outcomes.
Providing health data access to patients
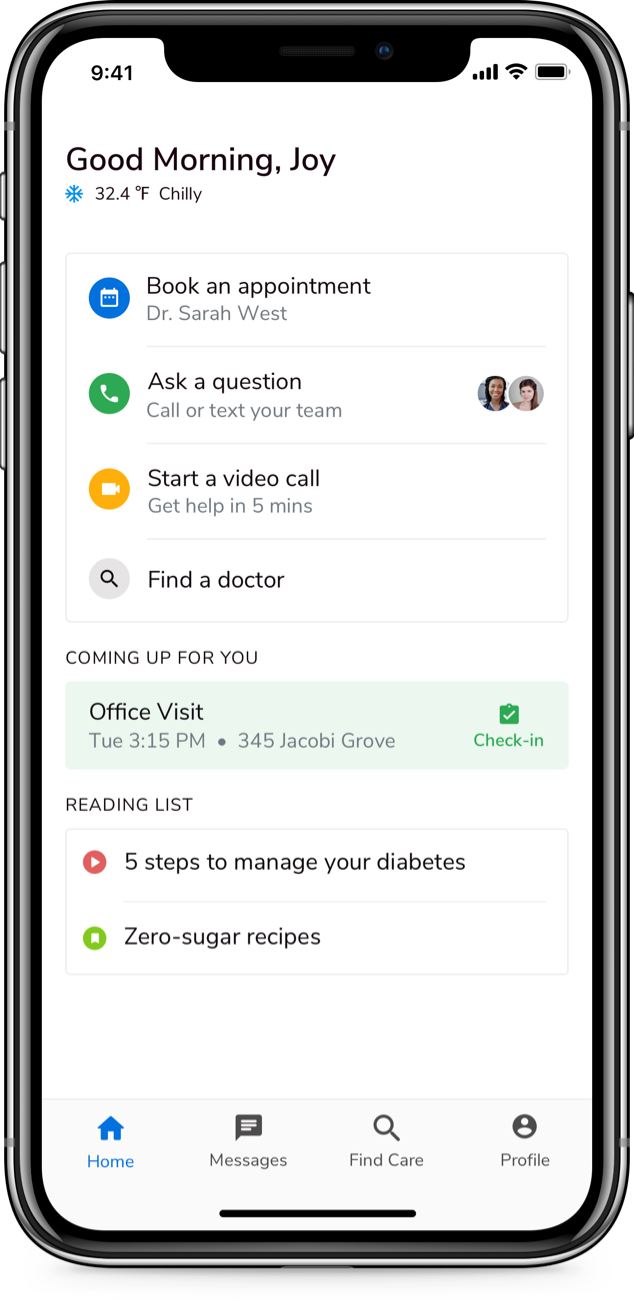
As the recipients of healthcare services, patients are entitled to get information about the cost, health plan coverage and healthcare services. However, due to technological barriers paired with an unwillingness to share control of the care journey, payers had not taken adequate steps to provide health data to the patient. Only recently, with ONC’s rule under the 21st Century Cures Act, it has become mandatory for payers to provide members with their electronic health information through third-party applications. To support patient access to health data, the rule has established requirements for secure, standards-based application programming interfaces (APIs).
“By requiring health insurers to share their information in an accessible format by 2020, 125 million patients will have access to their health claims information electronically,” said CMS Administrator Seema Verma.
In the coming years, the momentum of patient-centered care delivery will intensify. Getting providers and payers to work together to provide patients access to their healthcare data will substantially improve care and utilization management functions. Giving control of the healthcare journey to patients through a FHIR-enabled data platform will reduce the number of unnecessary tests and procedures and reduce the pressure on medical resources, thereby driving more efficiency in the healthcare system.
Establishing transparency in data exchange
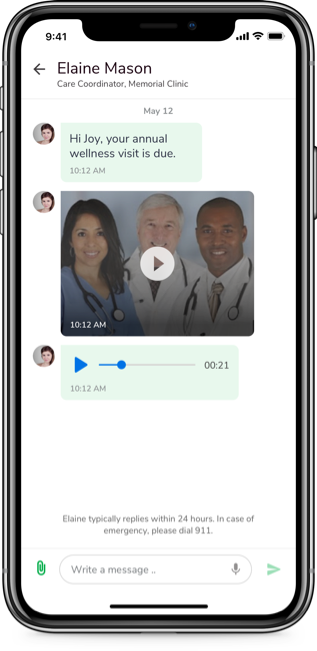
In many EHR contracts, providers are prohibited from sharing certain information related to the EHRs which includes screenshots or videos. In some cases, providers only perceive that they are not allowed to share such information, even though they don’t actually have a legal obligation if they do so. ONC’s final interoperability rule has laid out updated certification requirements that ensure that providers using certified health IT can share information about usability, user experience, security, and interoperability. Users of EHRs can even share videos and screenshots; however, there are still certain exceptions.
Previously, due to rigid contracts and the need to gain a competitive edge, there was a lack of transparency, which has cost the U.S. healthcare system dearly through the years. With ONC paving the way for increased transparency, health IT will improve operations and drive more efficiency in the coming years.
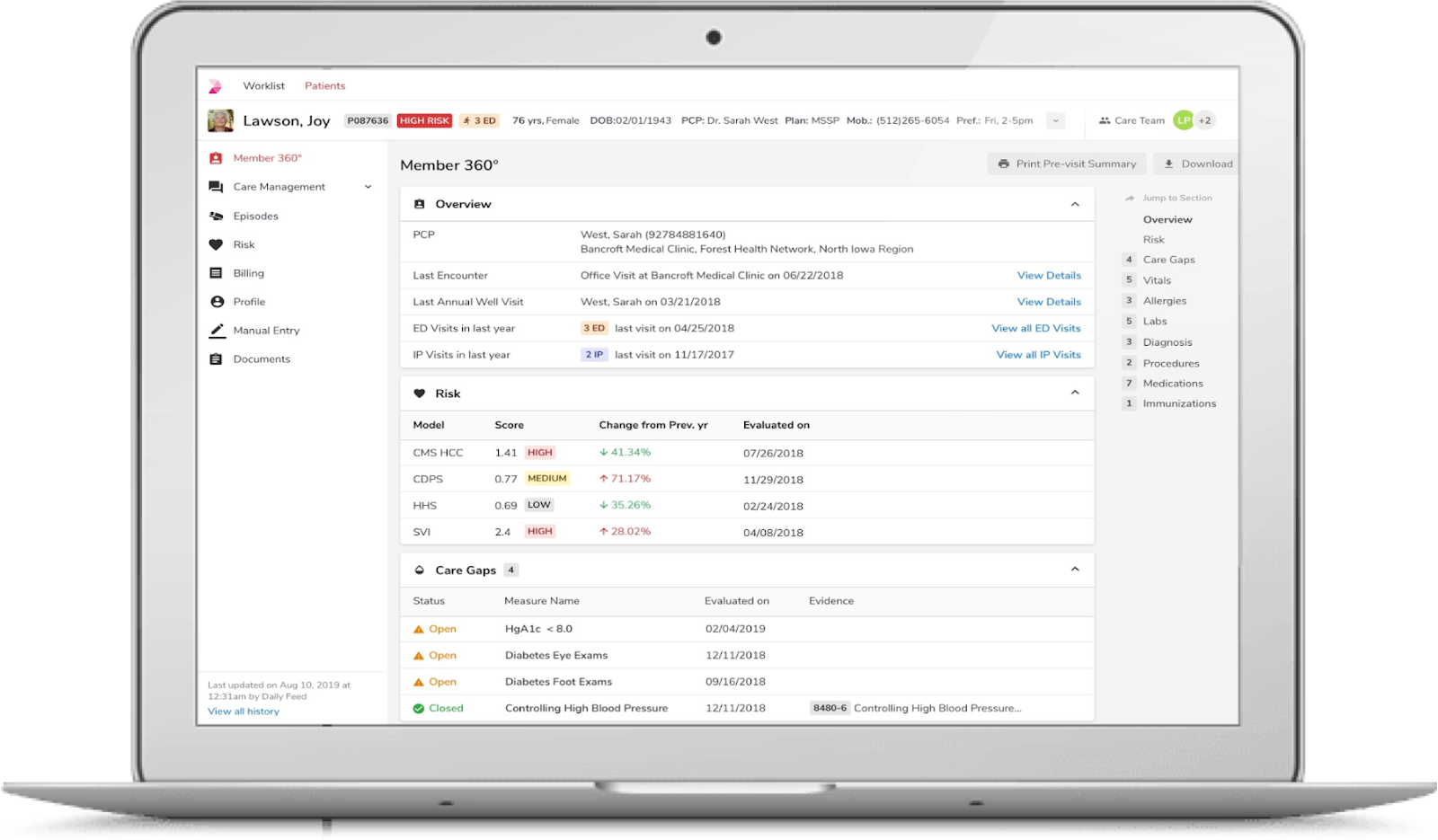
Data sharing through electronic notifications
Smooth exchange of patient data between different providers, practitioners, and facilities is also critical to providing excellent care delivery. The final ONC rule has mandated the adherence to new Conditions of Participation that enable better care coordination and improved outcomes. When a patient is admitted, transferred, or discharged, Medicare and Medicaid participating providers are required to share, through electronic notifications, the relevant data with the medical team assuming care of the patient. This will ensure timely care delivery, fewer “bounce back” admissions and medication errors, seamless follow-ups, improved outcomes, and, ultimately, patient satisfaction. While this has appeared as an interoperability mandate, it will benefit health plans and their provider networks, enabling them to achieve better results and reduce network leakage.
The road ahead
Healthcare consumerism is on the rise, and health plan beneficiaries want to receive the highest quality of care at reduced costs. By extending the health data pool to patients, the ONC final rule is handing over the reins of the care journey to the patients themselves. That way, quality and cost objectives will be fulfilled while accelerating the momentum of the value-based care movement.
CMS will add more fuel to this movement. Beginning on April 1, 2022, the states will have to share Medicare and Medicaid enrollment data with its beneficiaries daily. Not only will the accessibility of this data ensure better care coordination for the member population, but it will also allow patients to monitor the services they receive and the costs they incur. These rules will eventually weed out inefficient practices and establish cost transparency and fair competition in the healthcare space.

.svg)


.png)



.png)



.avif)


.png)
.png)
.png)




.svg)
.svg)

.svg)

