How can Healthcare Participants Tap into the Interoperability Opportunity with FHIR-enabled Data Activation Platform

Interoperability within the healthcare industry refers to the integration of information stored across multiple health systems and facilitates the easy exchange of, and access to, data. This leads to improved patient care throughout the healthcare continuum. A recent report stated that 84% of healthcare organizations did not have efficient access to needed information from exchange partners on a different electronic health record (EHR) in a way that helped them facilitate care across their network.
How does interoperability impact the healthcare industry?
The goal has always been to use data to optimize care by meeting the needs of the patient. Over the past decade, data has become digitized; however, the data deluge into electronic health record systems has also led to insufficient or siloed information for medical providers and networks. The needs of healthcare networks call for an information superhighway where participants can connect anytime and anywhere to obtain usable data. Hence, there is a strong interest in building the 'Internet of Healthcare' that connects the industry like never before.
The lack of interoperability has contributed to the onslaught of physician burnout, which has affected care at the most fundamental level. Nearly two-thirds of U.S. physicians feel burned out and distracted from their core mission of providing direct patient care. Missing bits and pieces of relevant information from different sources has further deprived them of a holistic view of their patient's profile, ultimately influencing the quality of care delivery and outcomes.
A wave of digitization could end healthcare's interoperability challenge
Like many other industries, healthcare can leverage modern technology powered by digitization to bid adieu to data challenges. While other industries have already benefited from the rise of technological advancements, healthcare clearly has some catching up to do.
Digital disruption, in any industry, comes in waves. Consider, for example, application programming interfaces or APIs. Today, consumer technology across many sectors such as the financial and travel industries runs on modern APIs. We have all heard that APIs play a big role in health IT interoperability, and with phrases such as "Blue Button 2.0" and "21st Century Cures Act," it's time we heard the real story behind APIs and determined the best way to move forward.
The importance of APIs and FHIR in healthcare
Application Programming Interface (API) is redefining the accessibility of information in the healthcare ecosystem. APIs enable seamless data exchange and flow across fragmented operations in the healthcare network. They are helping to provide safe and protected data reciprocity between the appropriate parties, not only ensuring the availability of relevant clinical information at the point of care but also delivering unified data to stakeholders for informed planning.
The HL7 Fast Healthcare Interoperability Resources (FHIR®) is a data standard developed by HL7, a healthcare IT standards body. FHIR uses uniform API standards and allows developers to create and customize plug-and-play applications. These applications can be plugged into any EHR and will feed information directly into the provider workflow, eliminating the gaps and pitfalls inherent in a document-based exchange. FHIR has a data-level access approach and offers visibility to even granular data.
What does FHIR mean for patients and providers?
Several federal agencies, including the Office of the National Coordinator for Health IT, have great expectations of FHIR. The instances and applications are limitless, and FHIR is set to counter significant challenges like improving patient engagement, developing robust care management programs, designing population health initiatives, and offering valuable insights at the point of care.
Several value-focused organizations and health IT vendors are using FHIR to expand their population health management approach. They can create specialty-specific information exchange programs that connect disparate data sources and offer real-time data access for providers to enhance clinical decision support. Along with improved patient engagement, reduced cycle time, and easy data exchange, providers can leverage FHIR to enable patient access to information under the guidelines of Meaningful Use and MACRA.
As for patients, FHIR solves the issue of having to negotiate multiple portals to contact and submit information to their healthcare providers. Situation-specific, granular FHIR programs can perform analytics on patient health information from EHRs, wearable devices, glucose monitors, and fitness trackers, and deliver a holistic view of all medications, episodes, and provider interactions. Patients are able to access this complete holistic record, share it among their providers, and interact with it to improve care management.
Latest interoperability rule implications on FHIR
The use of the HL7 FHIR Release 4 standard is mandatory under the new ONC rule. The certified API technologies will have to support FHIR Release 4.0.1. It is believed that the latest release standard of FHIR offers many improvements from the previous version. Nearly 3,000 changes have been made in the FHIR R2 to come up with the fourth release. FHIR R4 supports RESTful architectures and ensures seamless information exchange through digital documents and messages. Built on an evolutionary development path from the HL7 Version 2 and CDA, it allows their standards to co-exist and even support each other for improved quality and usage.
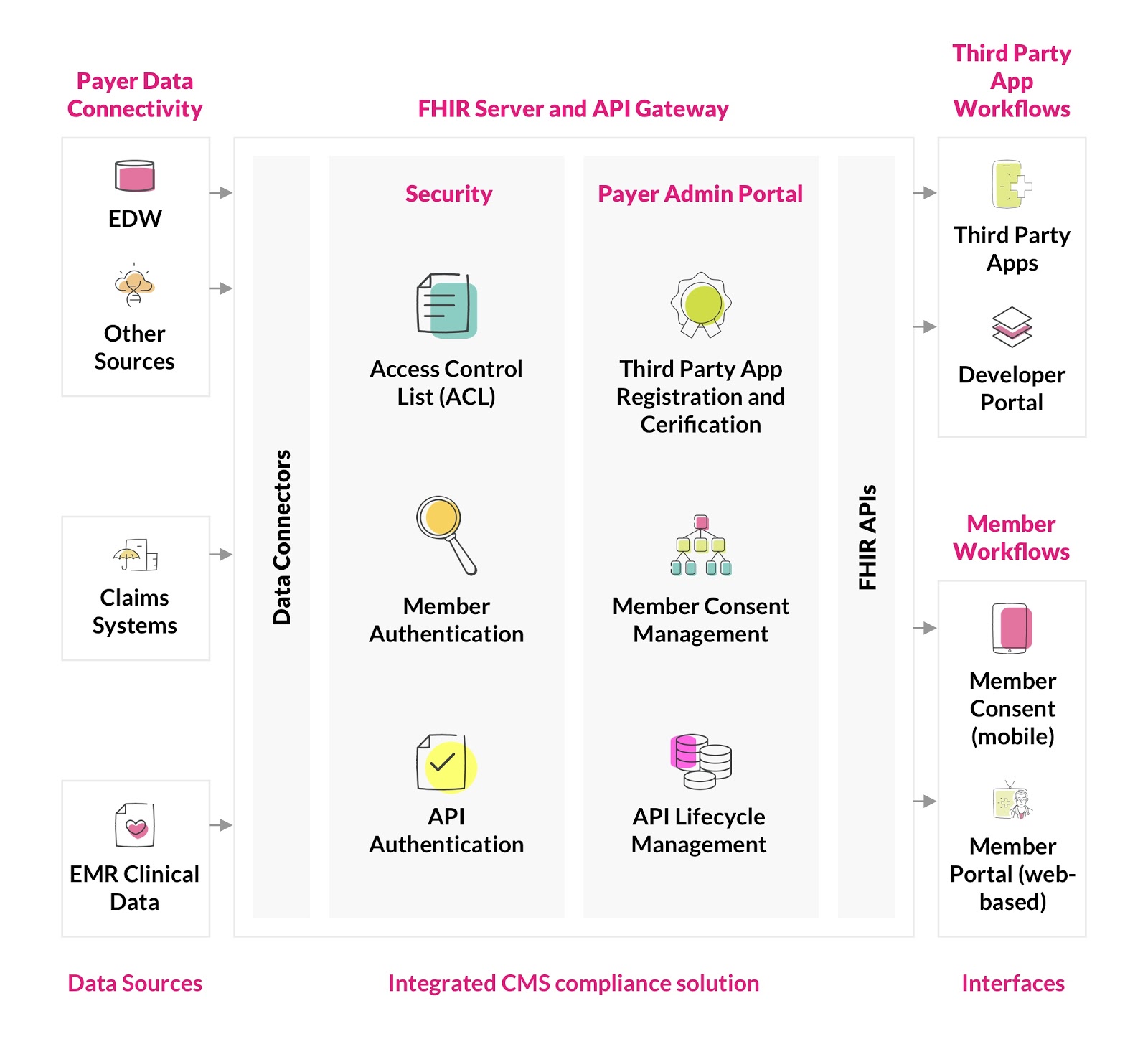
Innovaccer’s FHIR-enabled Healthcare Data Platform complies with the latest version, FHIR v4.0.1, and includes more than 400 search parameters and more than 800 analytical enrichments to clinical and claims data. The breadth of data that the platform provides allows it to serve as a foundation upon which custom applications can be designed and built by any healthcare organization.The platform provides a rich set of capabilities from scalable FHIR APIs, optimized FHIR data lake, a best-in-class API gateway, and cloud infrastructure, among other features.
The road ahead
Healthcare with APIs, in the long run, will become highly efficient and more effective. With patient participation in care planning, we can expect the advent of more economically sound and transparent procedures.
Once APIs expand completely into the healthcare space, and patients across the networks are empowered with access to their data, the entire healthcare ecosystem is bound to move more steadily towards improved utilization. APIs are our staircase to the goal of value-based care. With the potential to eliminate existing friction in healthcare cross-source operations, their implementation will surely lead to superior resource optimization and health outcomes.
To learn how to ensure compliance with the CMS interoperability rule and FHIR standards check out the industry’s most comprehensive Healthcare Data Platform for payers here.

.svg)


.png)



.png)



.avif)


.png)
.png)
.png)




.svg)
.svg)

.svg)

