LRx360
Specialty Pharmacy Platform Built to Transform Operational Performance, Clinical Outcomes, and Financial Results
Co-developed by Innovaccer and Longitude Rx, LRx360 transforms and unifies the patient and specialty prescription journey.
.png)
IN PARTNERSHIP WITH

Accelerate Access.
Recover Specialty Prescription Revenue.
Reduce Administrative Burden
Recover Specialty Prescription Revenue.
Reduce Administrative Burden
Completes Specialty Prescription Workflows Prospectively
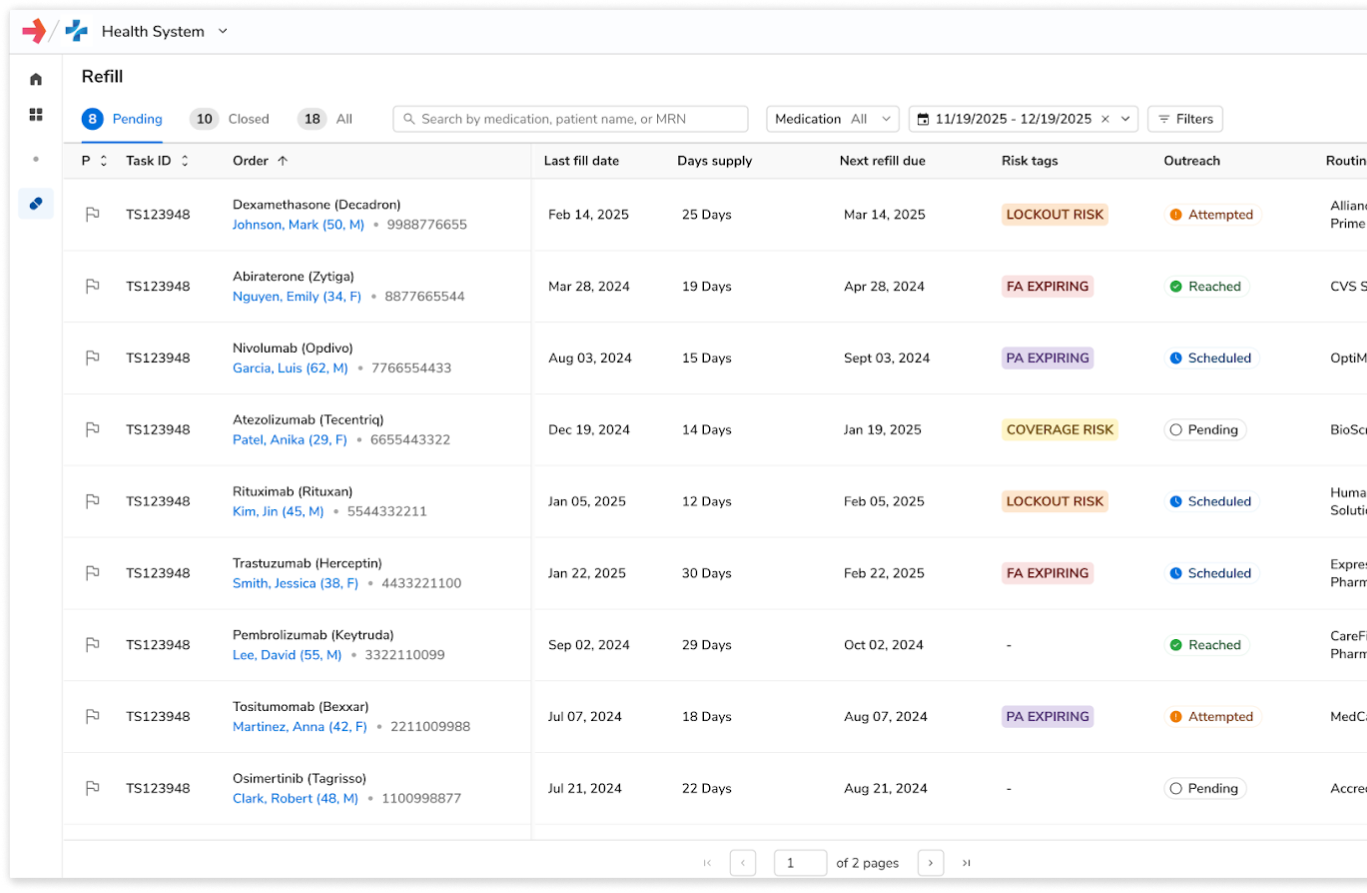
Reduce the rework- loop and avoid claim rejections by validating benefits and managing prior authorization prospectively
.png)
Protect Specialty Pharmacy Performance
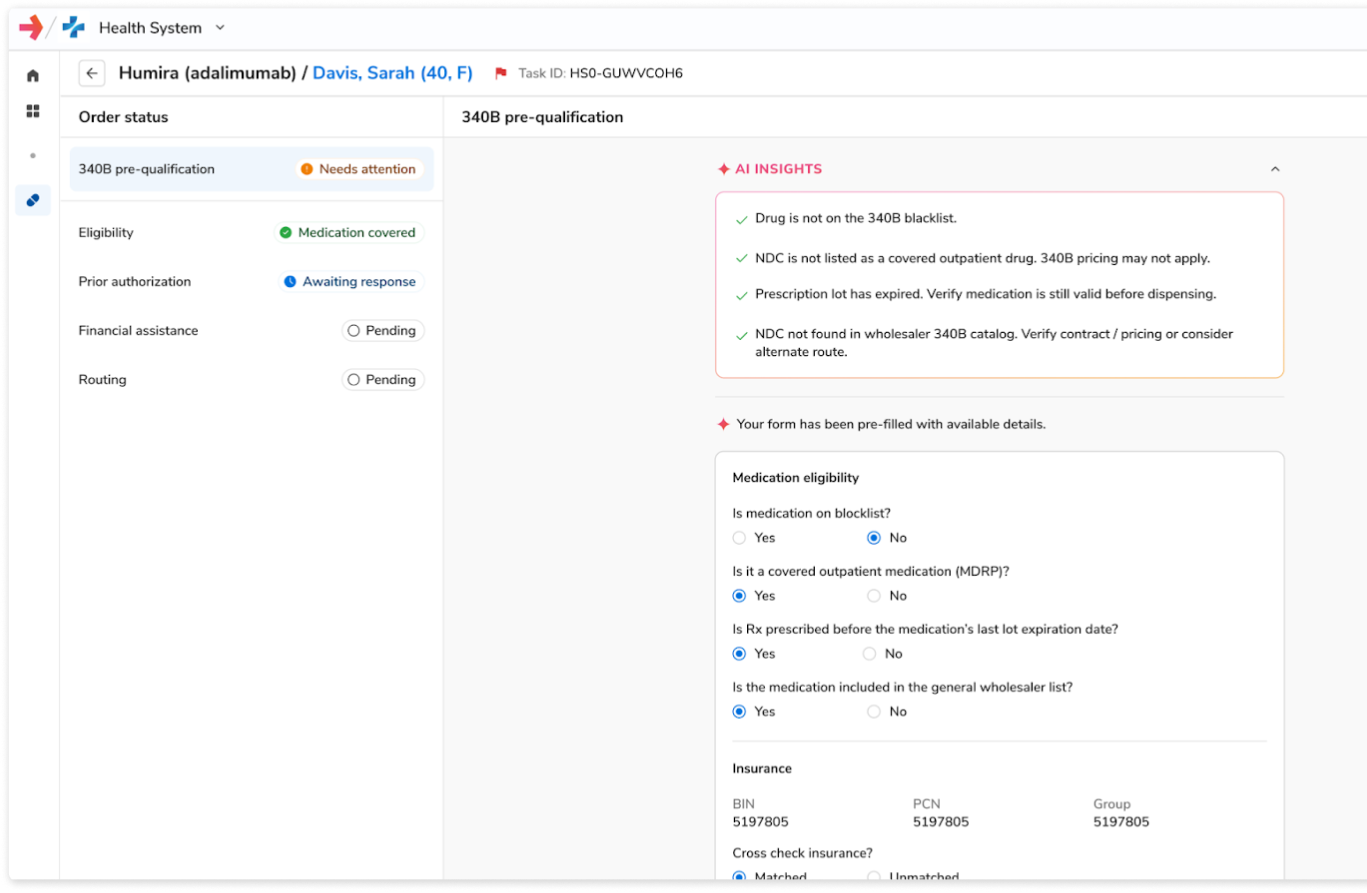
Purpose-built for 340B compliance, delivering modular capabilities for eligibility validation, exception management, and audit-ready reporting.

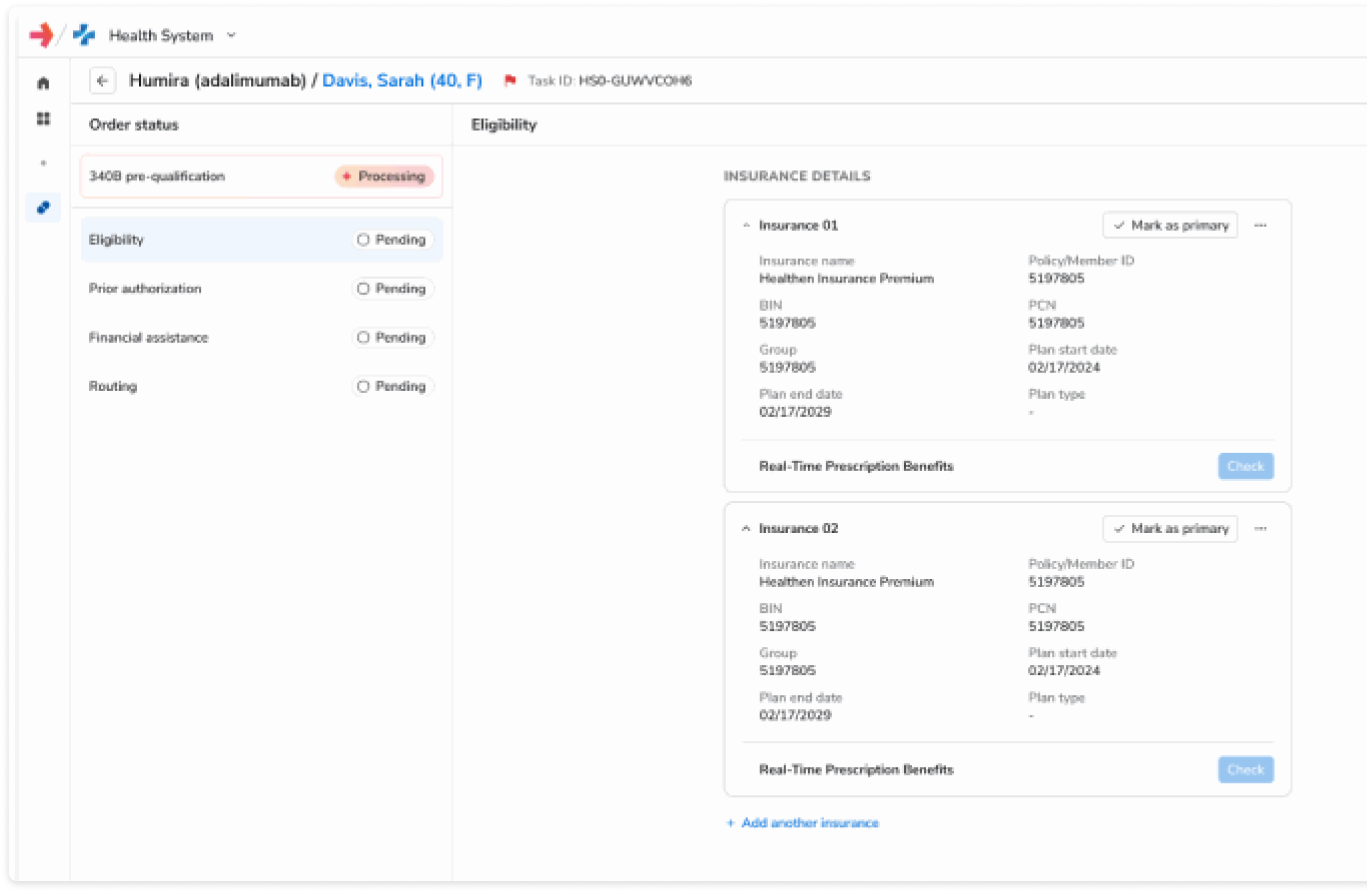
Orchestrate and Accelerate Time-to-Therapy
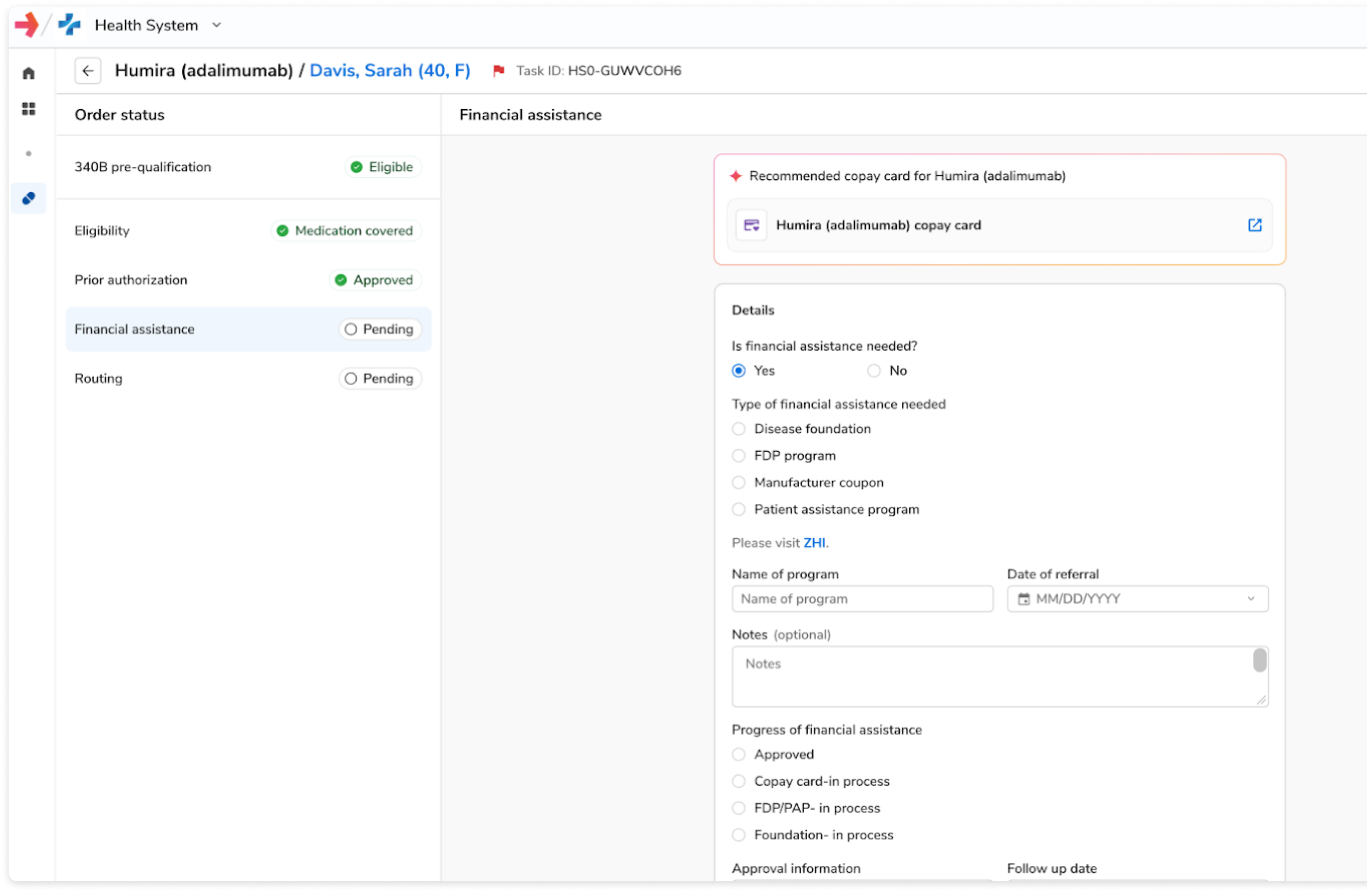
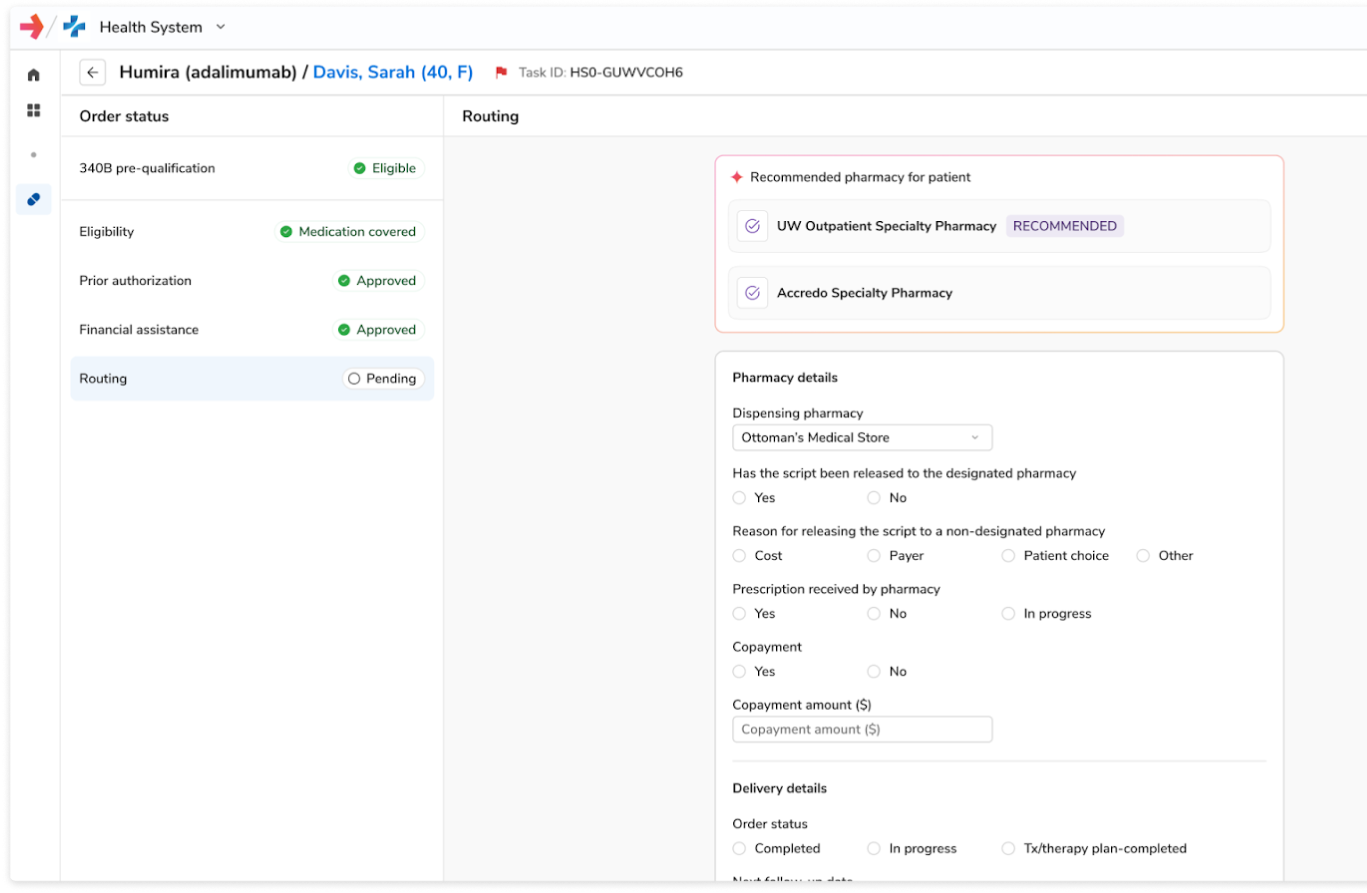
Complete benefits investigation, pharmacy and medical benefits prior authorization, financial assistance, and routing workflows, ensuring prescriptions can be filled without adding operational burden.
Ensure Continuity of Care and Measurable Outcomes
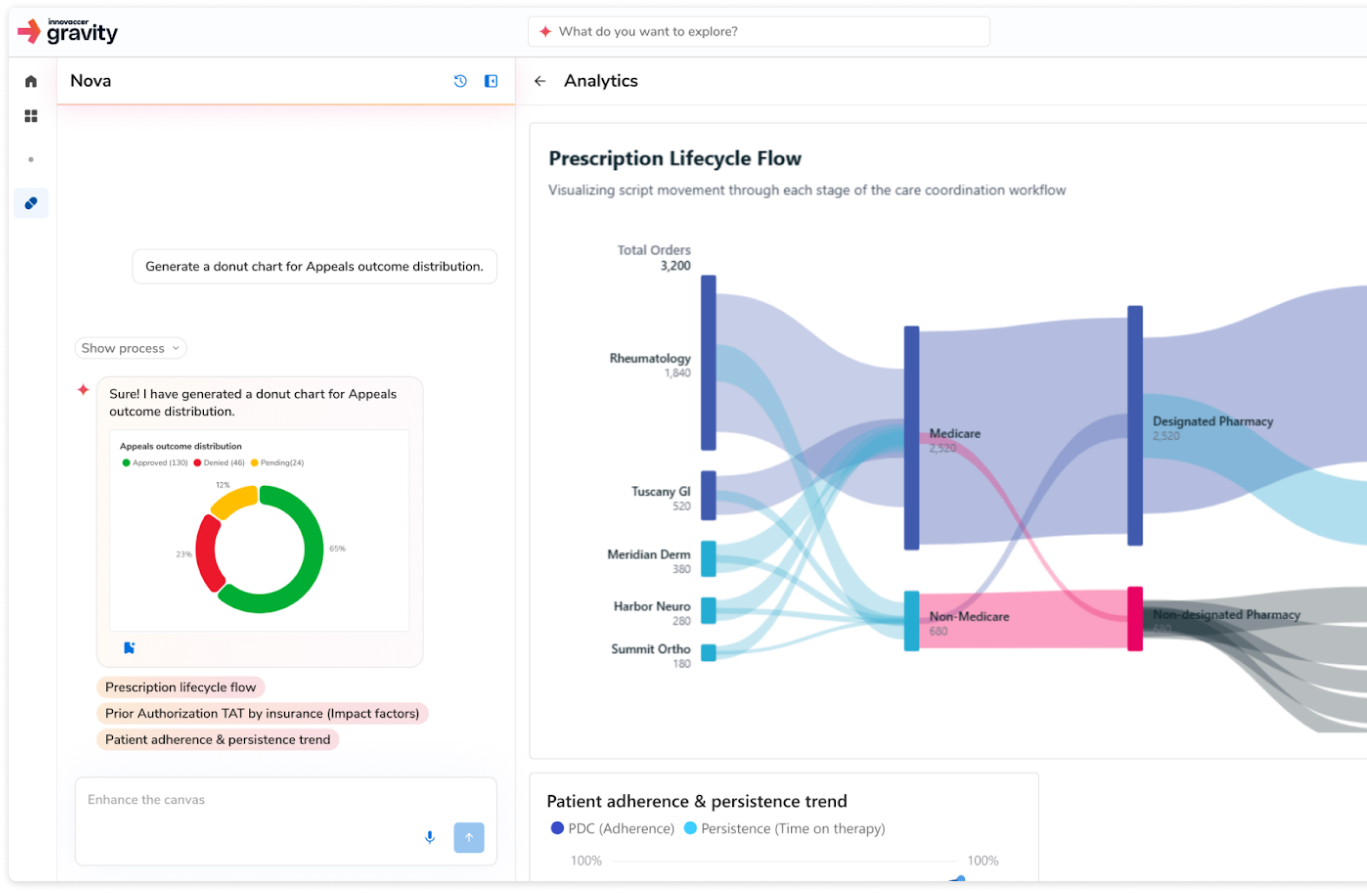
Turn operational efficiency into sustained patient and financial impact. Extend beyond operational automation to ensure patients start and stay on therapy.




.svg)


