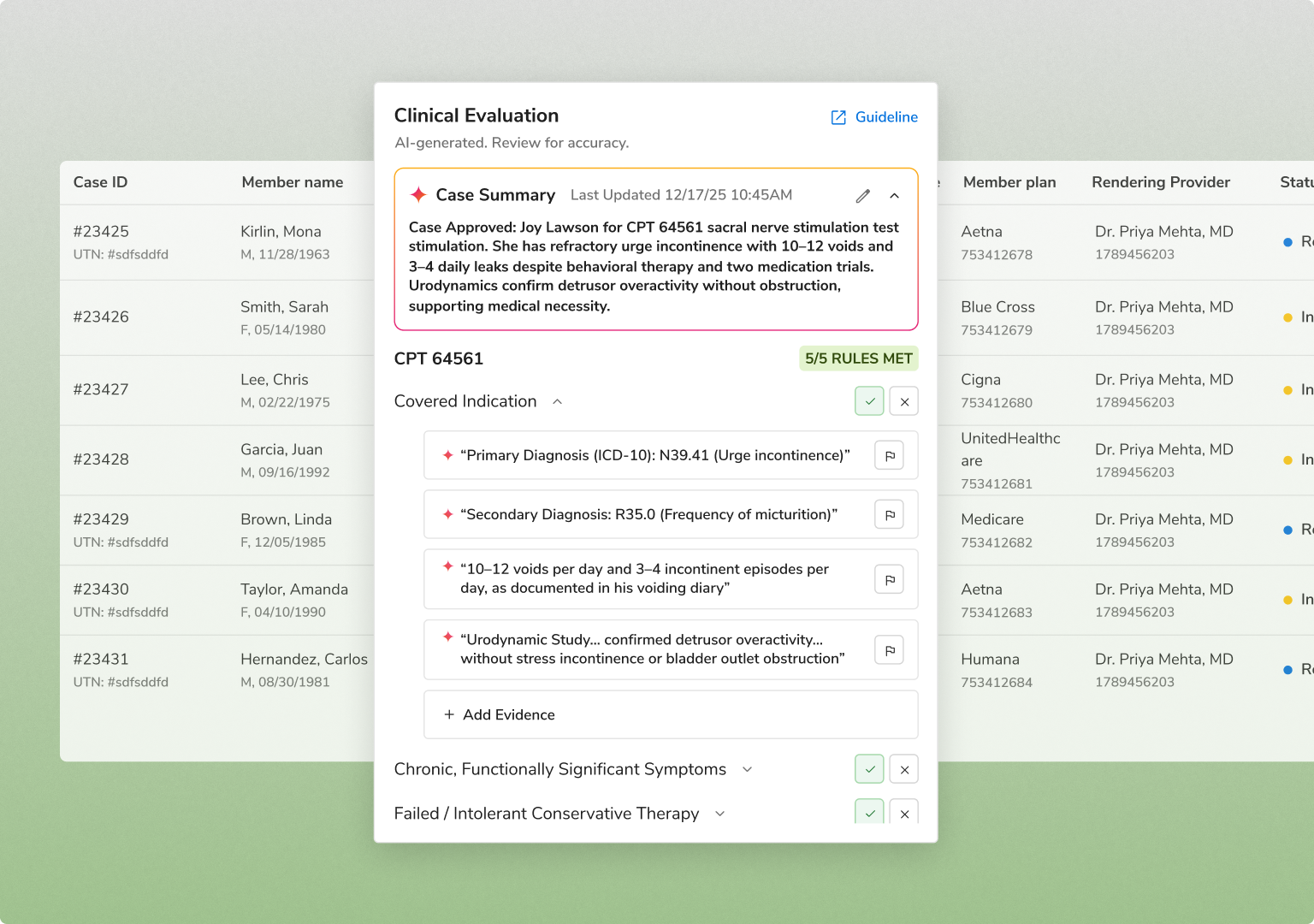
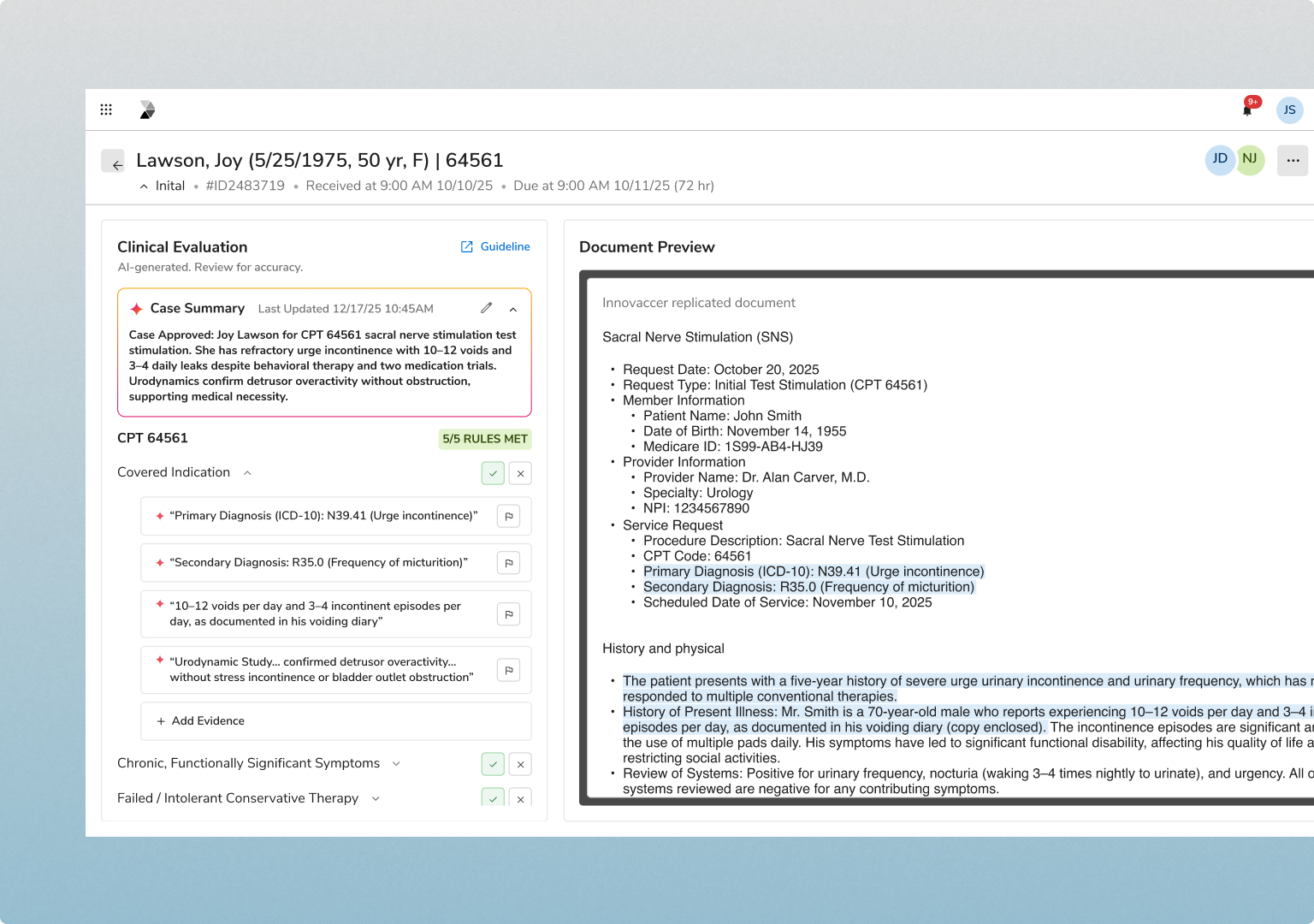
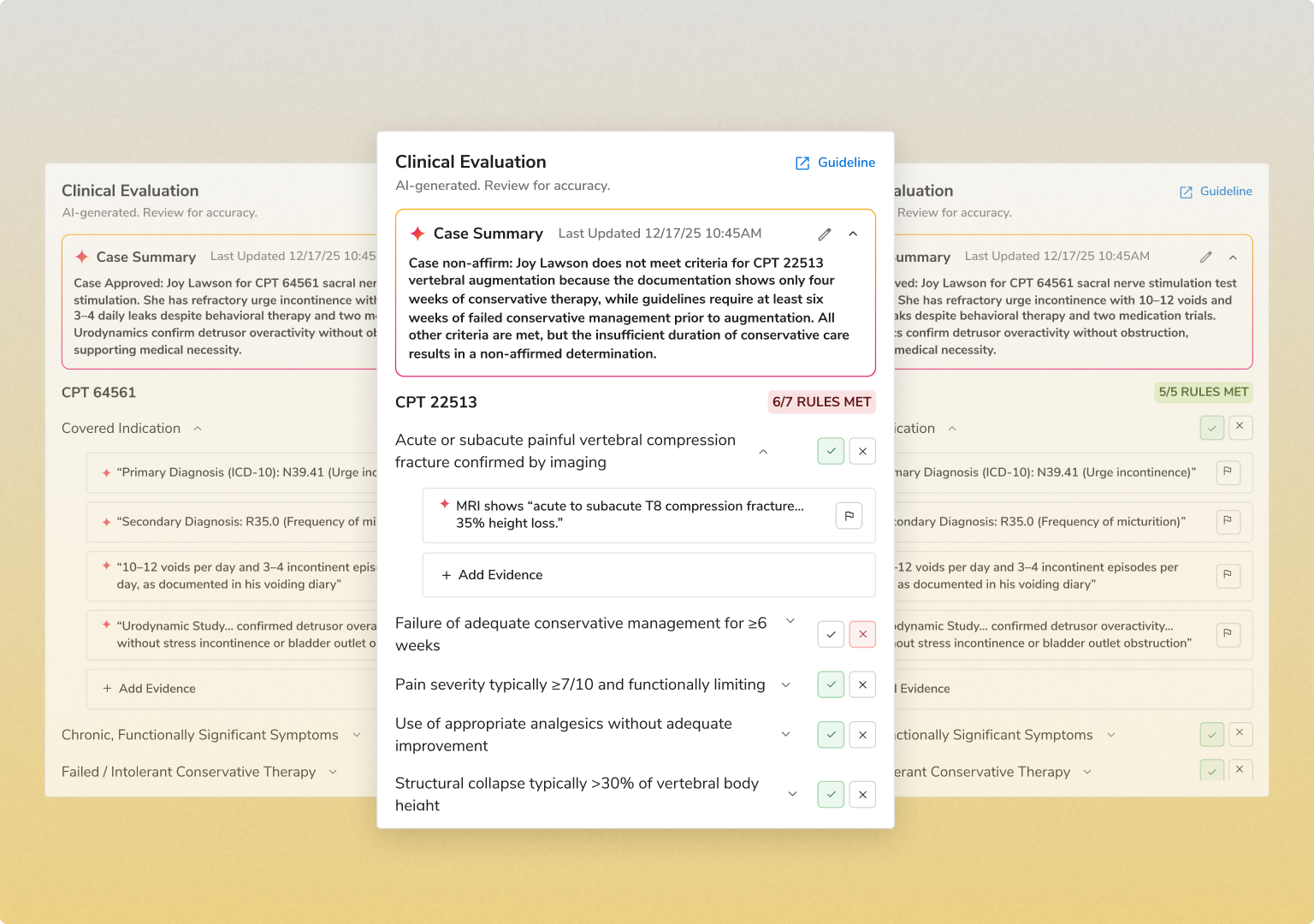
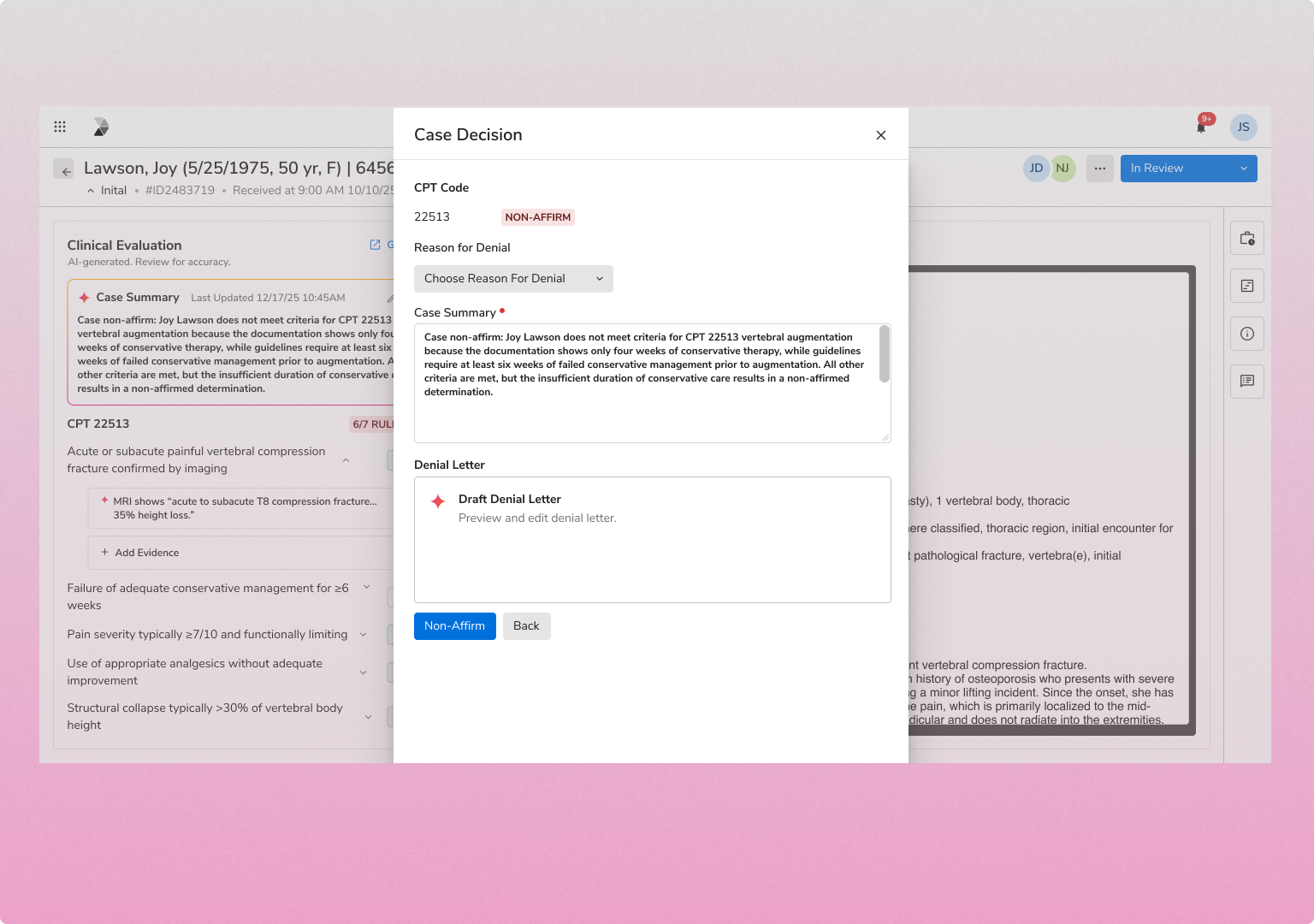
INTAKE & DATA EXTRACTION
Every request is captured and normalized across channels
FHIR API, provider portal, EDI X12 278, and fax/OCR
NLP extracts clinical evidence from unstructured documents
Eligibility verified at intake, with immediate tracking


.svg)





.svg)










“IInNote saves me 30 minutes a day that I would have otherwise spent chasing down information.”





.png)
.svg)
.svg)
.svg)
.svg)
.png)