Solving Coding Backlogs with Autonomous AI


Nearly every health system in the U.S. is wrestling with mounting medical coding backlogs—a problem that directly threatens revenue realization, compliance accuracy, and staff morale. Studies show that roughly one in five claim denials stem from coding errors, and more than half of these are never resubmitted, resulting in millions of dollars in lost reimbursement opportunities. These challenges are compounded by coder shortages and increasingly complex documentation requirements. Autonomous medical coding—AI-powered technology that automatically assigns, validates, and posts codes without routine human review—has emerged as a transformative solution. This article explores why traditional models fail to keep up and how autonomous AI platforms are reducing backlogs, increasing accuracy, and restoring financial velocity for modern health systems.
Challenges Contributing to Coding Backlogs in Health Systems
Persistent coding backlogs reflect a perfect storm of operational pressures: staffing limitations, surges in patient volumes, constantly evolving payer rules, and incomplete or inconsistent documentation. When claims pile up, denial rates climb and days in accounts receivable increase. For revenue cycle leaders, every day a chart goes uncoded represents delayed cash flow and heightened compliance risk. Addressing these compounding issues requires more than temporary staffing—it requires rethinking the workflow from data capture to code assignment.
Workforce Shortages and Turnover Impacting Coding Capacity
Workforce scarcity remains one of the most significant contributors to coding backlogs. The American Medical Association has reported a roughly 30% shortfall in the national medical coding talent pool. As veteran coders retire and new staff are hard to train, many health systems experience seasonal surges and persistent turnover that slow claims throughput. A recent AHIMA survey found that nearly half of respondents reported lower reimbursement rates and delayed claims directly linked to understaffing.
.png)
These pressures create a reinforcing cycle: coders face rising workloads, backlogs persist, and health systems lose revenue momentum.
Clinical Documentation and Coding Complexity as a Barrier
Even when staffing is stable, clinical documentation often remains incomplete or ambiguous. Missing signatures, unclear physician notes, or unstructured text in the EHR cause coders to issue queries and delay billing. As encounter types diversify—spanning multi-specialty inpatient stays to complex surgical episodes—coding complexity grows. This variability increases the potential for human error, driving up denials and rework. In many cases, the administrative lag sits not in data retrieval, but in the interpretation of complex clinical details.
Limitations of Traditional Computer-Assisted Coding Tools
Legacy computer-assisted coding (CAC) systems were built to accelerate manual workflows, not replace them. CAC generates code suggestions based on rules and patterns, but human coders must still validate and finalize each chart. This partial automation helps reduce keystrokes but doesn’t address the core backlog problem. While autonomous AI platforms—such as those integrated within Innovaccer’s Healthcare Intelligence Cloud—deliver four- to sevenfold productivity gains, CAC-based approaches yield far more modest improvements.

The takeaway: CAC alleviates some manual burden, but it’s ultimately constrained by its dependency on human verification.
Autonomous AI: Transforming Medical Coding Workflows
Autonomous AI represents a structural leap forward. These platforms perform full end-to-end coding by abstracting documentation, assigning codes, validating logic, and posting charges automatically for predefined encounter types—all with minimal human involvement. KLAS Research calls autonomous coding the top emerging AI use case in the revenue cycle. By removing routine human review, health systems can process charts in real time, cutting days off their billing cycle, increasing accuracy, and unlocking capacity for coders to focus on complex, high-value cases.
How Autonomous AI Differs from Traditional Coding Solutions
Autonomous medical coding isn’t just faster—it’s architected differently. These systems interpret clinical intent, not just keywords, producing finalized billing-ready codes that post directly into the EHR or financial system.
Definition: An autonomous medical coding platform uses AI to read, understand, and apply coding logic to complete encounters with no human action for standard chart types, while maintaining full auditability for oversight.
Key differentiators include:
- True end-to-end automation with human review reserved for exceptions
- Continuous learning models that adapt to payer rule changes
- Native integration into EHR workflows
- Configurable audit and compliance parameters
Innovaccer’s autonomous coding approach combines these differentiators with unified data integration, ensuring scalability and reliability across varied EHR environments.
Key Technologies Behind Autonomous Medical Coding
At the core of autonomous coding are AI techniques purpose-built for healthcare language and regulatory precision:
- Natural language processing (NLP): Enables understanding of unstructured clinical notes to identify diagnoses, procedures, and context.
- Machine learning (ML): Continuously improves coding accuracy by learning from historical patterns and human feedback.
- Predictive analytics: Anticipates documentation gaps or coding discrepancies before submission.
Unlike rule-based CAC systems, autonomous AI applies clinical language understanding modules that interpret meaning rather than rely on keyword matching—yielding higher precision and audit confidence.
Benefits of Autonomous AI in Reducing Coding Backlogs
Health systems adopting autonomous AI report striking performance improvements:
- Up to 70% of coding tasks automated by 2030 projections
- Denial rates reduced from 18% to 3%, saving millions annually
- Coding accuracy reaching 97% versus traditional averages below 90%
- Productivity gains of 4–7x across targeted specialties
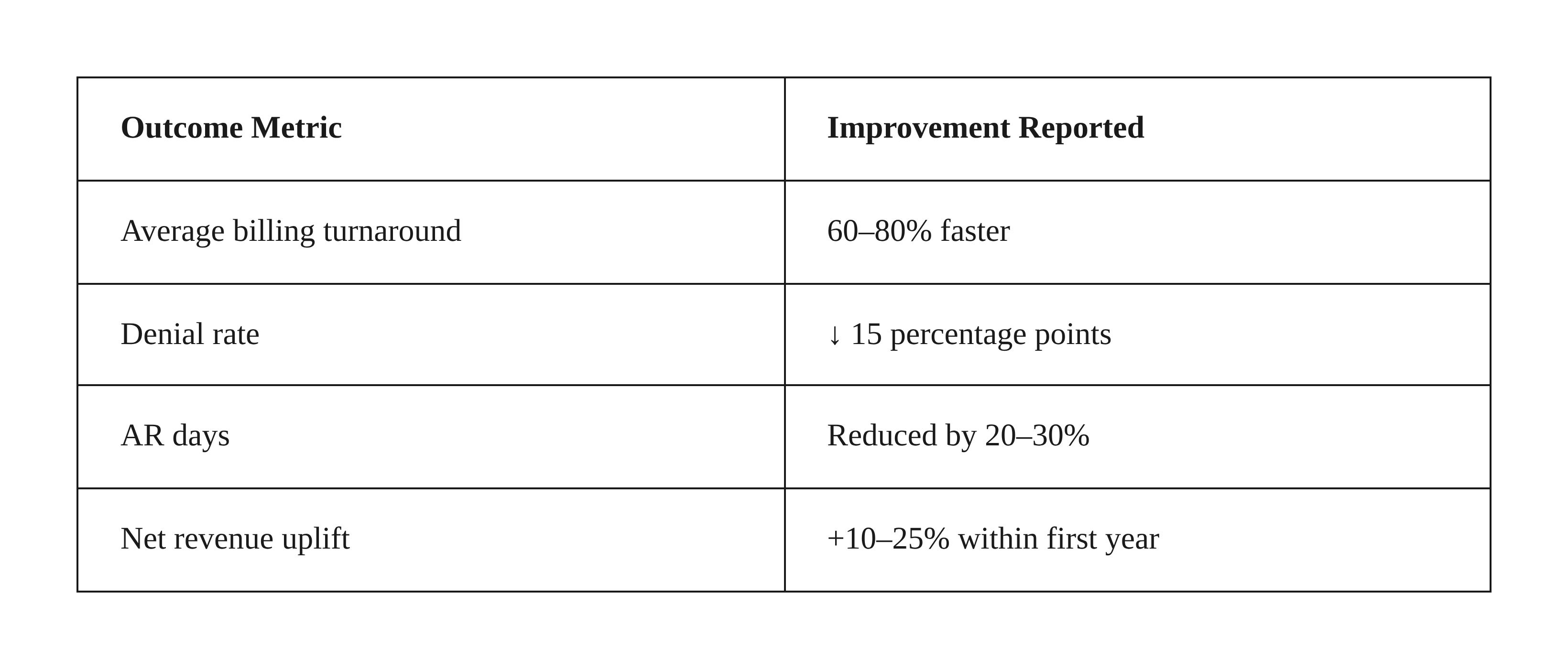
These numbers translate directly into accelerated cash flow, fewer rebillings, and a rebalanced workforce.
Real-World Outcomes and Financial Impact of Autonomous Coding
Validated implementations show substantial financial and operational gains:
- One regional clinic halved coding time and increased revenue by 25% after AI implementation.
- A large integrated system reported $504 million in incremental revenue after deploying an autonomous platform across service lines.
- Another organization achieved a 23% net revenue lift per patient after optimizing coding accuracy through AI.
When scaled across enterprise operations, these impacts transform the revenue cycle from reactive to predictive.
Strategic Considerations for Implementing Autonomous AI in Coding
For health systems preparing to adopt autonomous coding, success begins with a deliberate, phased approach:
- Start with predictable, structured specialties like emergency department, pathology, or radiology.
- Define outcome-based KPIs—turnaround time, denial rate, coder productivity.
- Ensure strong EHR integration for seamless code posting.
- Implement audit dashboards for transparency and compliance.
- Invest in change management—train coders to manage exceptions and quality audits.
Collaborating with data and workflow integration partners like Innovaccer can help ensure that autonomous coding aligns with enterprise data governance and interoperability goals.
Balancing Automation with Human Expertise for Coding Integrity
Autonomous AI doesn’t eliminate the need for coders—it elevates their role. Routine encounters can be managed by AI at volume, allowing coders to focus on nuanced cases, audits, and denial prevention. This human-AI partnership ensures automation enhances accuracy and speed while preserving the human judgment essential for clinical and regulatory alignment.
Building Trust, Compliance, and Transparency in Autonomous Coding
Compliance leadership requires visibility, and autonomous platforms are designed accordingly. They maintain complete audit trails, provide explainable coding rationales, and align with payer rules to ensure continuous regulatory readiness.
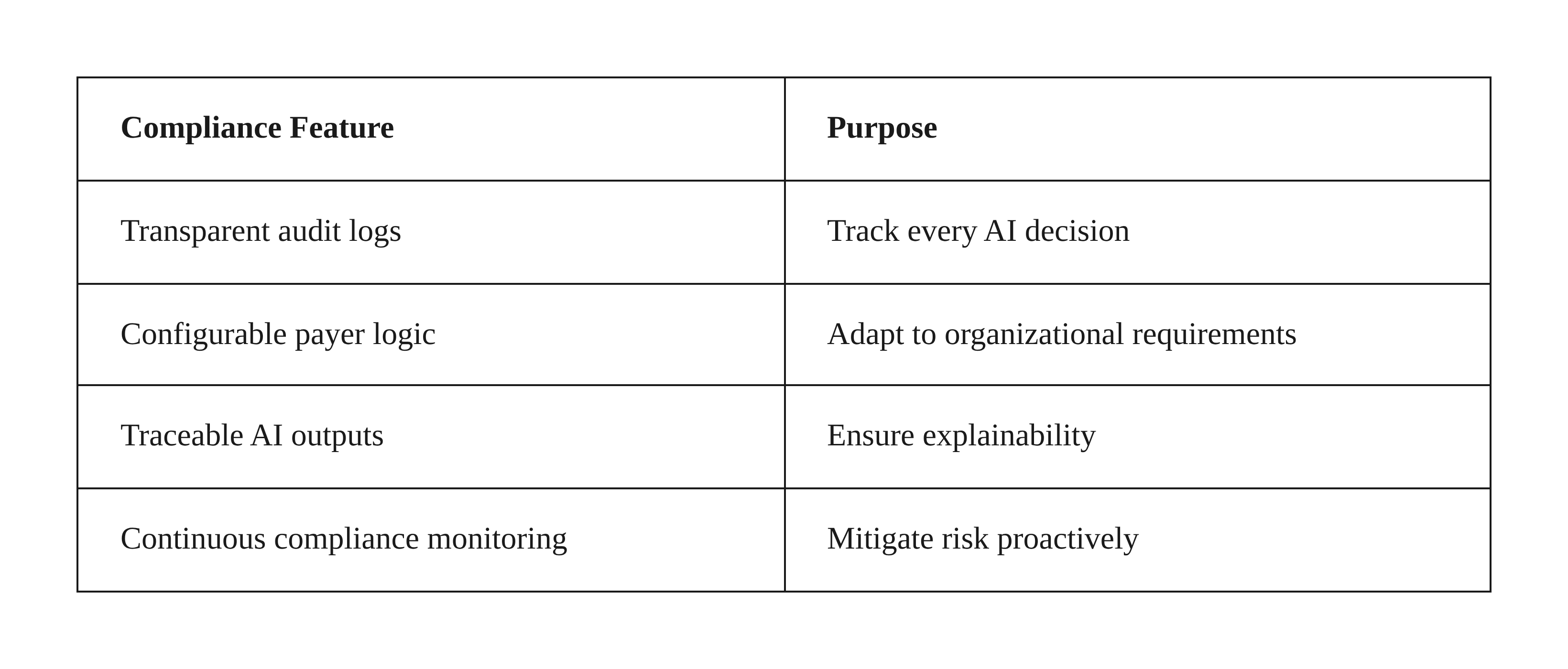
Compliance-ready autonomous coding means every automated decision can be audited, reviewed, and traced back to its clinical source.
Future Trends and the Role of Autonomous AI in Health System Growth
Autonomous coding is rapidly becoming a cornerstone of the intelligent revenue cycle. As models extend into complex inpatient coding and integrate more tightly with EHRs, they will not only eliminate backlogs but actively optimize revenue integrity in real time. Looking ahead, predictive analytics and cross-department data unification will enable systems—like those powered by Innovaccer’s Healthcare Data Platform—to drive measurable ROI, accelerate transformation, and support scalable value-based care strategies.
Frequently Asked Questions
What are the main causes of coding backlogs in health systems?
Coding backlogs stem from staff shortages, incomplete documentation, complex coding requirements, and fluctuating patient volumes that manual workflows can’t easily absorb.
How does autonomous AI reduce denials and improve coding accuracy?
By automating code assignment, validation, and posting, autonomous AI identifies documentation gaps before submission—significantly reducing denials and improving accuracy.
When should health systems consider adopting autonomous coding solutions?
Health systems should explore autonomous coding when coder shortages, rising denials, or chronic backlogs threaten financial performance and operational efficiency.
What financial benefits can health systems expect from autonomous coding?
By accelerating billing and improving first-pass accuracy, autonomous coding can deliver substantial revenue uplift and measurable reductions in A/R days.
How do autonomous coding systems ensure compliance and auditability?
They offer complete audit trails, payer-aligned logic, and explainable coding decisions to maintain transparency, compliance, and trust across workflows.
For more insights on AI-driven revenue transformation, explore Innovaccer’s Healthcare Intelligence Cloud and AI-powered documentation solutions.

.svg)


.png)



.png)



.avif)


.png)
.png)
.png)



.svg)
.svg)

.svg)

